Journal About Dental Insurance Guide

Source: ladylesliebelize.com
Welcome to Dental Insurance Guide — a resource designed to explain dental insurance in a clear and practical way. Our goal is to help readers understand how dental coverage works, what dental insurance typically covers, and how different plans affect the cost of dental care.
In our journal, we publish guides covering topics such as individual dental insurance, dental insurance with no waiting period, Medicare and Medicaid dental coverage, and dental insurance for adults, seniors, and self-employed individuals. We also explain important insurance concepts including deductibles, annual maximums, waiting periods, claims processing, and reimbursement policies.
Our articles explore common dental procedures and how insurance may apply to them, including implants, braces, crowns, dentures, root canals, wisdom teeth removal, dental bridges, and routine cleanings. We also explain how costs may vary with or without insurance and how coverage can differ between providers and plan types.
Read more

Top Stories

Read more

Read more

Read more

Read more
Trending

Read more

Read more
Latest articles








Most read

Read more

Read more
In depth
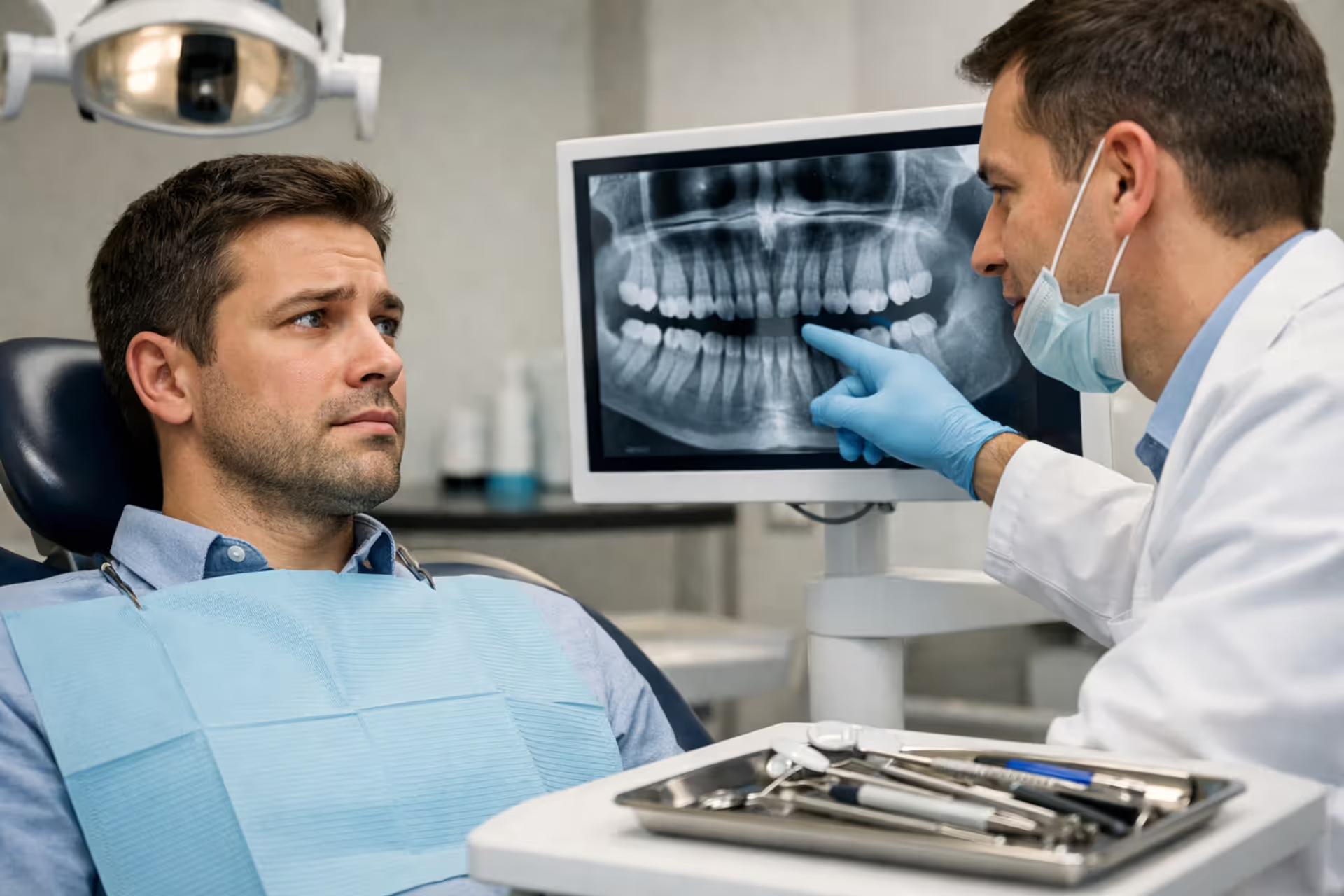
When you're sitting in the dentist's chair and they mention needing x-rays, your first thought is probably "what's this going to cost me?" If you've got dental insurance, you're looking at around $10-$50 coming out of your pocket for standard imaging. No coverage? That bill jumps to anywhere from $25 to north of $300, depending on what type of pictures your dentist needs to take.
Here's why that gap exists: insurance companies treat most routine x-rays as preventive care, which means they'll pick up 80-100% of the tab once you've cleared your deductible. But—and this is a big but—your actual costs swing wildly based on things like your plan's annual caps, how long you've been covered, and whether you're seeing someone in your insurance network.
The specifics of what you'll pay depend on multiple moving parts in your coverage. Your plan documents spell out which imaging procedures qualify for full coverage versus partial reimbursement, and those details make the difference between a $15 copay and a $100 surprise bill.
Average Cost of Dental X Rays by Type
Not all dental x-rays are created equal. The imaging your dentist orders depends on what they're trying to see. A quick bitewing that spots cavities hiding between teeth runs you far less than a 3D scan that maps every millimeter of your jawbone.
Let's break down what different procedures actually cost:
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.