
A person holding a dental insurance card in front of a blurred modern dental office with a dental chair and equipment in the background
What Is Dental Insurance and How Does It Work
Content
Content
Dental insurance helps Americans manage the cost of oral healthcare by covering a portion of routine and restorative dental services. Unlike medical insurance, dental plans operate on a separate system with distinct coverage tiers, annual maximums, and cost-sharing structures. Understanding these mechanics can save you hundreds or thousands of dollars annually while maintaining better oral health.
Understanding Dental Insurance Basics
Dental insurance is a type of health coverage designed specifically to reduce out-of-pocket costs for dental care. Most plans work by paying a percentage of your dental bills after you meet certain requirements, such as staying within a network of approved dentists or paying an annual deductible.
The primary purpose of dental insurance is to encourage preventive care—regular cleanings, exams, and X-rays that catch problems early when they're less expensive to treat. A small cavity detected during a routine checkup might cost $150 to fill, while waiting until it requires a root canal and crown could run $2,500 or more.
Dental insurance remains separate from medical insurance for historical and practical reasons. In the 1950s, dental benefits emerged as standalone offerings because oral health was viewed as distinct from general medicine. Even today, dentists and physicians operate under different licensing systems, use separate billing codes, and follow different treatment protocols. This separation means you'll typically have two insurance cards—one for your doctor and one for your dentist—even if they're offered by the same insurance company.
Most dental plans share common features: monthly premiums (the amount you pay to maintain coverage), annual deductibles (what you pay before insurance kicks in), and annual maximums (the most your plan will pay in a calendar year). These maximums typically range from $1,000 to $2,000 per person, which hasn't increased much since the 1980s despite rising dental costs.

Author: Olivia Davenport;
Source: ladylesliebelize.com
How Dental Insurance Works
When you purchase dental insurance, you pay a monthly premium regardless of whether you visit the dentist. For employer-sponsored plans in 2026, employees typically pay $15 to $50 per month for individual coverage, with employers covering the rest. Individual market plans run higher, often $30 to $80 monthly depending on your location and coverage level.
After paying premiums, you'll encounter a deductible—usually $50 to $100 per person annually. This deductible applies only to certain services. Most plans waive the deductible for preventive care, meaning your cleanings and exams cost nothing out-of-pocket if you visit an in-network dentist.
The network distinction matters significantly. In-network dentists have contracted with your insurance company to accept negotiated fees. If your dentist charges $200 for a filling but has agreed to accept $120 from your insurer, you benefit from that $80 discount even before insurance pays its share. Out-of-network dentists can bill their full rates, and your insurance may reimburse a smaller percentage or use a different fee schedule, leaving you with substantially higher costs.
Coinsurance percentages determine how much you pay versus what your insurance covers. A plan with 80% coinsurance for basic procedures means the insurance pays 80% of the approved amount and you pay the remaining 20%. If that filling costs $120 (the negotiated rate), you'd pay $24 while insurance covers $96.
The annual maximum caps your benefits at a set dollar amount per calendar year. Once your insurance has paid out $1,500 (a common maximum), you're responsible for 100% of any additional dental costs until January 1st when your benefits reset. This ceiling catches many people off guard when they need extensive work—a single crown can consume half your annual maximum, leaving little coverage for other procedures.
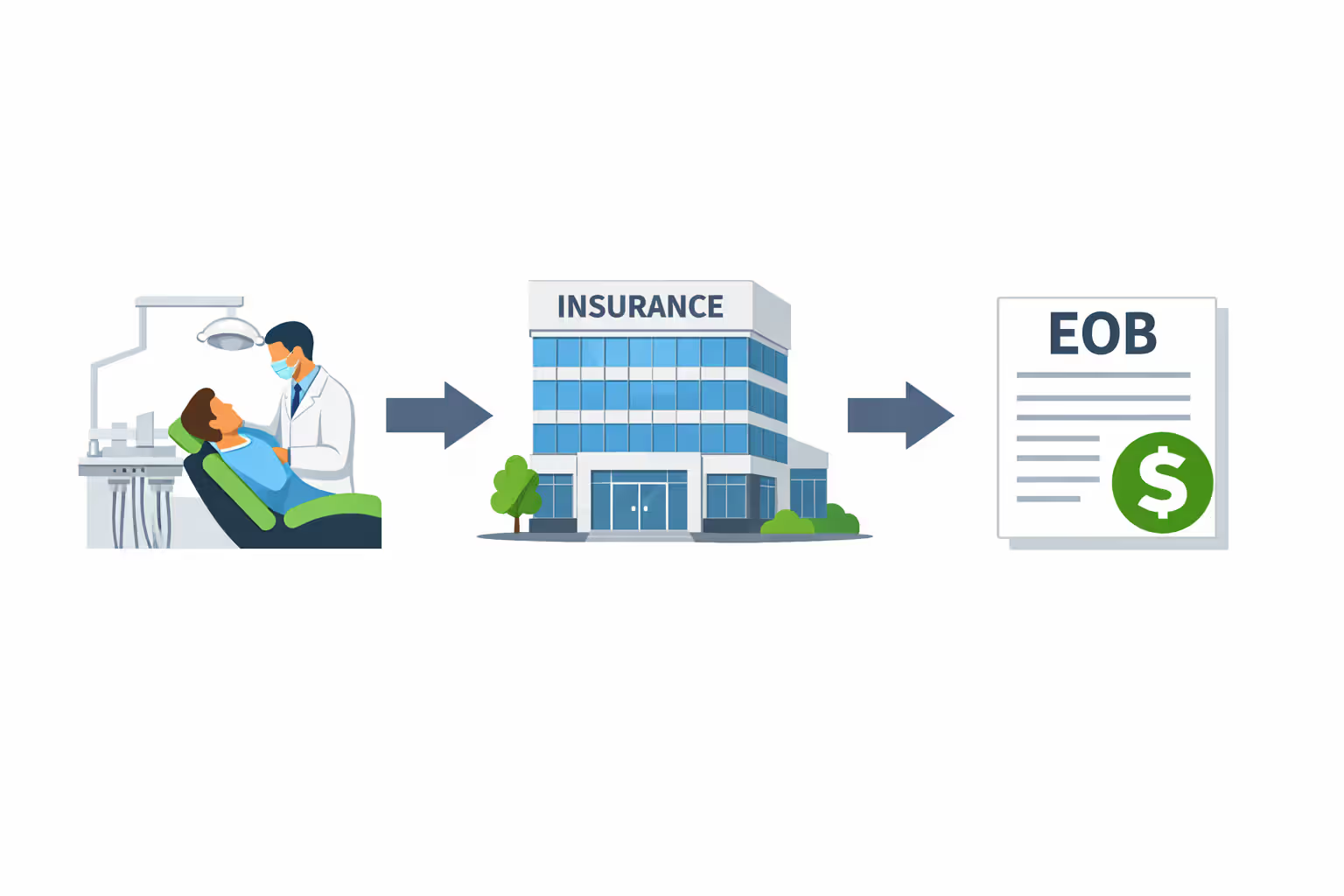
The claim process typically happens behind the scenes. Your dentist's office submits claims electronically to your insurance company, which processes them and sends payment directly to the dental practice. You receive an Explanation of Benefits (EOB) showing what was billed, what the insurance paid, and what you owe. Some offices require payment upfront and reimburse you after insurance pays, while others bill you only for your portion after receiving insurance payment.
Author: Olivia Davenport;
Source: ladylesliebelize.com
Types of Dental Insurance Coverage
Most dental insurance plans organize services into three tiers based on complexity and cost. This tiered structure, often called the 100-80-50 model, determines how much your plan pays for different types of care.
Preventive Care
Preventive services receive 100% coverage under most plans with no deductible. This category includes routine cleanings (typically two per year), comprehensive oral exams, routine X-rays, fluoride treatments for children, and sealants. Some plans also cover periodontal maintenance cleanings for patients with gum disease history at the preventive level.
The logic behind full preventive coverage is straightforward: catching problems early saves money. An insurer would rather pay $100 for a cleaning that identifies a small cavity than $2,000 for an emergency root canal six months later when that cavity has infected the tooth's pulp.
Basic Procedures
Basic procedures typically receive 70% to 80% coverage after you meet your deductible. This tier includes fillings, simple extractions, non-surgical periodontal treatments like deep cleanings (scaling and root planing), and emergency care for pain relief.
The 20% to 30% you pay out-of-pocket for basic work adds up. A filling might cost you $30 to $60, while a deep cleaning in all four quadrants of your mouth could run $200 to $300 after insurance. These costs remain manageable for most budgets, which is why insurers cover the majority but still require cost-sharing to discourage unnecessary procedures.
Major Procedures
Major procedures receive 50% coverage in most plans, meaning you split the cost evenly with your insurance company. This category includes crowns, bridges, dentures, implants (when covered), root canals, and oral surgery beyond simple extractions.
The 50% coinsurance on major work means significant out-of-pocket costs. A crown typically costs $1,000 to $1,500, so you'd pay $500 to $750. Multiple crowns or a bridge can quickly exhaust your annual maximum, leaving you to cover 100% of additional costs. This is where many people discover the limitations of dental insurance—it helps but doesn't eliminate major expenses.
Author: Olivia Davenport;
Source: ladylesliebelize.com
What Does Dental Insurance Typically Cover
Dental insurance covers a broad range of services, though coverage levels vary by procedure type. Understanding what's included helps you maximize your benefits and avoid surprises.
Diagnostic and preventive services form the foundation of coverage. Semi-annual cleanings and exams are standard, with most plans allowing one comprehensive exam and two routine cleanings per year. Bitewing X-rays (the small X-rays that check for cavities between teeth) are typically covered once yearly, while full-mouth X-rays are covered every three to five years. Children often receive additional preventive coverage, including fluoride treatments through age 14 or 18 and sealants on permanent molars.
Restorative procedures like fillings receive basic coverage. Most plans cover amalgam (silver) fillings at the negotiated rate but may cover tooth-colored composite fillings only up to the cost of amalgam, requiring you to pay the difference if you choose the more aesthetic option for back teeth.
Endodontic treatments such as root canals fall under either basic or major coverage depending on your plan. Front teeth (anterior) root canals sometimes receive better coverage than molars because they're less complex. Apicoectomies (surgical root canal procedures) typically fall under major coverage.
Periodontal treatments for gum disease start with scaling and root planing (deep cleanings), usually covered as basic procedures. Ongoing periodontal maintenance cleanings may be covered as preventive care, though some plans limit you to a combined total of cleanings rather than allowing both regular and periodontal maintenance visits.
Prosthodontic services like crowns, bridges, and dentures receive major coverage. Plans often distinguish between different crown types—full metal crowns may be covered at 50% while porcelain-fused-to-metal or all-ceramic crowns might have higher patient cost-sharing. Dentures and bridges typically require pre-authorization, meaning your dentist submits a treatment plan for approval before beginning work.
Oral surgery coverage depends on complexity. Simple extractions are usually basic procedures, while surgical extractions, impacted wisdom teeth removal, and jaw surgery fall under major coverage. Some plans require complex oral surgery to be billed through your medical insurance rather than dental coverage.
Common exclusions include cosmetic procedures like veneers placed solely for appearance, teeth whitening, and cosmetic bonding. Adult orthodontics rarely receives coverage, and when child orthodontics are covered, there's typically a separate lifetime maximum of $1,000 to $1,500. Implants remain controversial—some plans cover them as major procedures while others exclude them entirely, considering them elective or cosmetic.
Common Dental Insurance Plan Types
Dental insurance comes in several formats, each with different rules about provider choice, costs, and flexibility. Choosing the right type depends on your priorities and circumstances.
| Plan Type | Average Monthly Premium | Provider Flexibility | Referral Required | Out-of-Network Coverage | Best For |
| PPO | $30-$60 | High – any dentist | No | Yes, reduced benefits | Those who value choice and have a preferred dentist |
| HMO/DHMO | $15-$30 | Low – network only | Sometimes | No | Budget-conscious individuals willing to change dentists |
| Indemnity | $40-$80 | Highest – any dentist | No | Yes, same benefits | Those prioritizing maximum freedom and willing to pay more |
| Discount Plan | $10-$20 | Medium – network only | No | No | Healthy individuals needing only preventive care |
PPO (Preferred Provider Organization) plans dominate the dental insurance market. They offer networks of dentists who've agreed to discounted fees, but you can visit any dentist you choose. Staying in-network maximizes your benefits because you get both the negotiated discount and higher coinsurance percentages. Going out-of-network means paying higher fees and receiving lower reimbursement percentages, but you're not locked into specific providers. PPOs work well if you've established a relationship with a dentist who accepts your insurance or if you want flexibility when traveling.
HMO or DHMO (Dental Health Maintenance Organization) plans require you to choose a primary care dentist from a limited network. All care must go through this dentist, and you may need referrals to see specialists. In exchange for these restrictions, HMOs offer lower premiums and often lower copays with no deductibles or annual maximums. The catch: if your assigned dentist doesn't suit your needs or you move outside the service area, switching can be complicated. HMOs make sense for families on tight budgets who don't mind network restrictions.
Indemnity plans (also called traditional or fee-for-service plans) are becoming rare but offer maximum flexibility. You can visit any dentist anywhere, and the insurance reimburses a percentage of the dentist's actual charges or a set fee schedule, whichever is lower. You typically pay the dentist upfront and submit claims for reimbursement. Higher premiums and more paperwork are trade-offs for complete freedom. These plans appeal to people who travel frequently or live in areas with limited dental networks.
Discount dental plans aren't insurance but membership programs. You pay an annual or monthly fee to access discounted rates at participating dentists—typically 10% to 60% off standard fees. There are no claims, deductibles, or annual maximums because you're simply getting pre-negotiated discounts. These work for people with minimal dental needs or those using them to supplement insurance that's exhausted its annual maximum. The downside: you're still paying most costs out-of-pocket, just at reduced rates.

Author: Olivia Davenport;
Source: ladylesliebelize.com
What Dental Insurance Doesn't Cover
Understanding dental insurance limitations prevents frustration and financial surprises. Several common restrictions apply across most plans.
Waiting periods delay coverage for certain services after you first enroll. Basic procedures might have 3 to 6-month waiting periods, while major procedures often require 6 to 12 months of continuous coverage before benefits apply. Preventive care typically has no waiting period. These delays prevent people from buying insurance only when they need expensive work, then canceling after treatment. If you're shopping for coverage and know you need a crown, factor in that you might wait a year before insurance helps pay for it.
Pre-existing conditions may face coverage limitations. If you're already in active treatment for a dental issue when you enroll, some plans won't cover completing that treatment. For example, if you've started a root canal but haven't finished it, your new insurance might not pay for the crown that completes the procedure. This varies by plan and state regulations, so review policy documents carefully.
Cosmetic dentistry receives no coverage under standard dental insurance. Veneers placed to improve appearance, professional whitening, and cosmetic bonding are out-of-pocket expenses. The line blurs when cosmetic work also serves functional purposes—a crown on a front tooth after an accident might be partially covered even though it improves appearance, because it also restores the tooth's function.
Experimental or investigational treatments are typically excluded. New technologies or procedures not widely accepted by the dental community won't receive coverage until they become standard of care. This can include certain laser treatments, alternative implant systems, or novel restorative materials.
Annual and lifetime maximums create hard coverage ceilings. Once you've used your $1,500 annual maximum, you're self-paying until the next calendar year. Some plans also impose lifetime maximums on specific services—orthodontics commonly has a one-time $1,500 lifetime benefit, meaning after that's exhausted, you'll never receive orthodontic coverage under that plan again.
Frequency limitations restrict how often certain procedures are covered. Most plans allow cleanings every six months, X-rays annually or every few years, and crowns on the same tooth only once every five to seven years. If your crown fails after three years, insurance won't pay for a replacement—you're responsible for the full cost because you haven't met the frequency requirement.
Age restrictions apply to some preventive services. Fluoride treatments and sealants often have age cutoffs, typically covering children but not adults. Some plans extend these benefits through age 18 or 19, while others stop at age 14.
The biggest misconception about dental insurance is that it works like medical insurance with comprehensive coverage. In reality, dental insurance is more of a maintenance plan that helps with routine care and offsets some major expenses, but it won't eliminate large bills the way medical insurance can after you hit your out-of-pocket maximum. I tell my patients to think of it as a coupon book that makes regular care affordable and provides a discount on bigger procedures, not as complete financial protection
— Dr. Jennifer Martinez
Frequently Asked Questions About Dental Insurance
Dental insurance serves as a cost-management tool rather than comprehensive financial protection. The annual maximums that haven't kept pace with inflation mean you'll still face substantial out-of-pocket costs for major dental work, but consistent preventive care covered at 100% can prevent many expensive problems from developing.
Maximize your benefits by using your preventive visits every six months—these cost you nothing beyond premiums and catch problems while they're small and inexpensive to fix. Schedule major work strategically, splitting procedures across calendar years when possible to access two years of annual maximums. If you need $3,000 in dental work and your plan has a $1,500 maximum, completing half in December and half in January could save you $1,500 compared to doing everything in one year.
Review your plan's specific coverage details annually, as benefits can change. Understand your deductible, coinsurance percentages, annual maximum, and any waiting periods or frequency limitations. Keep your insurance card accessible and confirm your dentist remains in-network before major appointments.
For those facing significant dental needs that exceed insurance coverage, ask your dentist about payment plans, health savings accounts (HSAs), or flexible spending accounts (FSAs) that let you use pre-tax dollars for dental expenses. Some dental offices offer in-house financing or work with third-party healthcare credit companies.
Dental insurance works best when you view it as a partnership—you maintain good oral hygiene and attend preventive appointments, while insurance helps manage costs when problems arise. This approach keeps your teeth healthy and your dental expenses predictable and manageable over the long term.
Related Stories
Read more
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.




