Dental office chair with insurance document on a side table in a bright modern clinic
What Is a Dental Insurance Deductible?
Content
Content
Your dental insurance deductible is the dollar amount you must spend from your own pocket on covered services before your insurance carrier begins to share the costs with you. This differs from your monthly premium payment, which you provide to the insurance company whether you visit a dentist or not—the deductible only becomes relevant when you actually receive treatment that falls into certain coverage categories.
The majority of dental plans organize benefits into three distinct tiers: preventive, basic, and major services. Your deductible generally kicks in for basic work like cavity fillings and tooth extractions, plus major treatments such as dental crowns or root canal therapy. Preventive care—your twice-yearly cleanings and checkup exams—usually skips the deductible requirement altogether, which means your plan pays for these services right from your first appointment without you needing to reach any threshold first.
Grasping how the deductible mechanism operates helps you forecast your dental spending and select insurance coverage that matches both your oral health requirements and your financial capacity.
Understanding Your Dental Insurance Deductible
When discussing what a deductible for dental insurance means, we're talking about a specific dollar threshold you need to satisfy before your insurance company begins paying its portion of eligible treatment costs. This threshold restarts every year, most commonly on January 1st or on the anniversary date when your policy originally took effect, depending on whether you have an employer plan or individual coverage.
The deductible functions differently from other ways you share costs with your insurer. Your monthly premium maintains your active coverage—it never reduces what you owe toward your deductible. A copayment is a set dollar amount you provide at each appointment for particular services, and these fixed fees don't reduce your deductible either. Coinsurance represents the percentage split you pay after satisfying your deductible; for instance, when your policy pays 80% of a filling once you've met the deductible, you handle the remaining 20%.
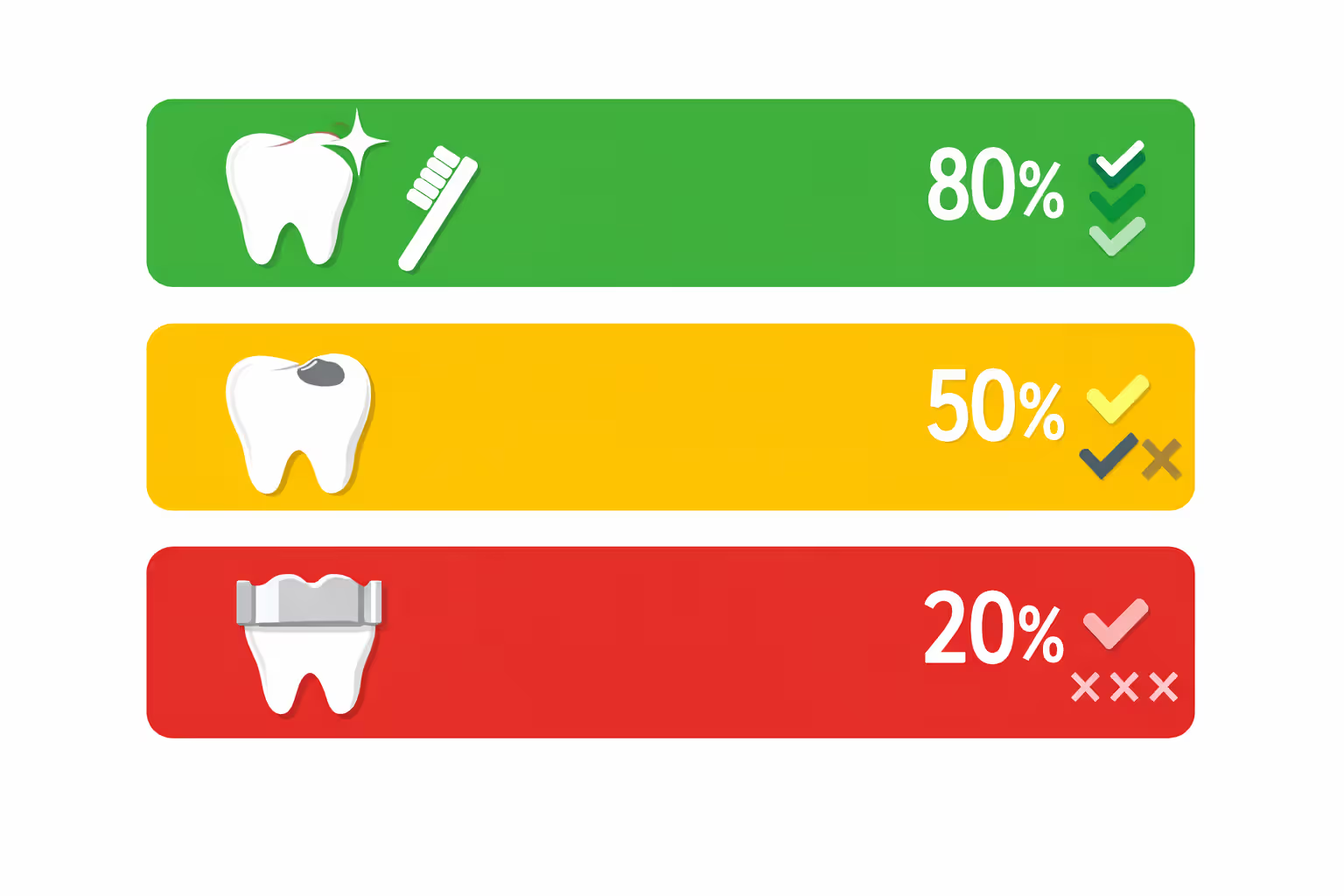
Different service categories interact with your deductible in distinct ways:
Preventive services (cleanings, examinations, diagnostic X-rays): Insurance companies cover these at 100% without requiring any deductible payment. You schedule your cleaning, sit in the chair, get your teeth polished, and leave without opening your wallet beyond the premiums you already pay monthly.
Basic procedures (cavity restorations, routine tooth removals, gum disease treatments): Your deductible applies to this category. Say you carry a $50 deductible and require a filling priced at $200. You cover the initial $50, and then your coinsurance percentage determines how you split the remaining $150 with your insurance company.
Major procedures (crowns, bridgework, dentures, endodontic treatment): The deductible requirement extends to these services as well. Once you've satisfied your deductible through either basic or major treatment earlier in the year, your plan's coinsurance formula determines your cost responsibility for any additional procedures during that benefit period.
A frequent source of confusion: satisfying your deductible doesn't trigger 100% insurance coverage for everything afterward. After you've cleared the deductible hurdle, you continue paying coinsurance—typically somewhere between 20% and 50% based on the procedure category and your particular policy terms.
Author: Olivia Davenport;
Source: ladylesliebelize.com
How Dental Insurance Deductibles Work in Practice
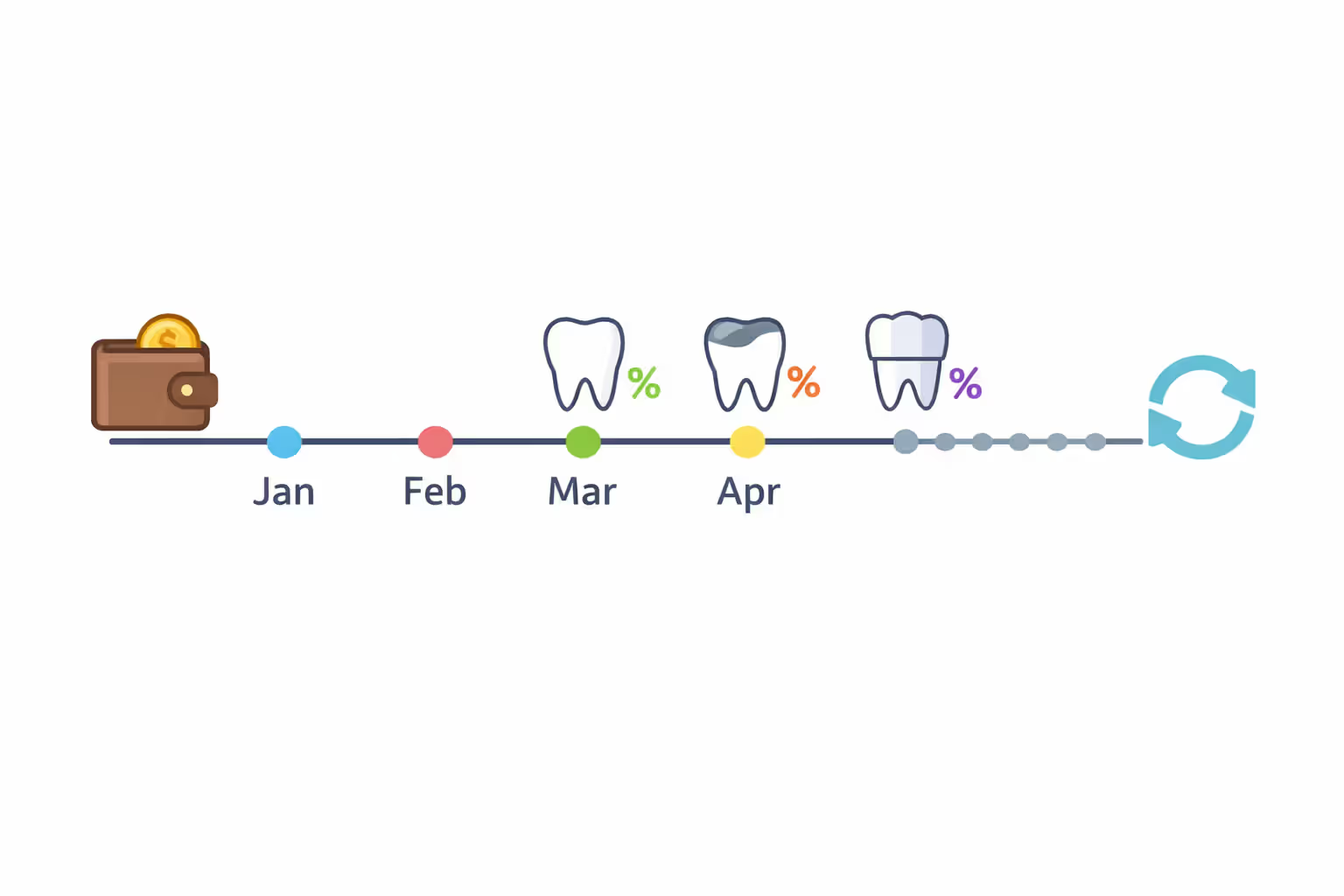
Your dental insurance deductible returns to zero at the start of each new benefit period. For the vast majority of employer-provided plans and individual marketplace policies, this refresh happens on January 1st. Some coverage tied to a company's fiscal calendar or your specific enrollment date might reset according to different schedules, so verify this detail in your benefits documentation.
Insurance policies distinguish between per-person and family-wide deductible structures. An individual deductible applies separately to each covered person—every family member needs to satisfy their own amount before their coverage benefits activate. A family deductible operates under different logic: when the total qualifying expenses from all covered household members combined reach a predetermined sum (frequently two to three times what one person's deductible would be), the insurance begins covering costs for every family member, including those who haven't yet reached their personal deductible amount.
Let's walk through a practical example: Sarah carries dental coverage with a $50 per-person deductible and 80% coinsurance for basic work. In March, she requires two fillings with a combined cost of $350. She pays her $50 deductible upfront. The remaining $300 becomes subject to coinsurance—her insurance pays 80% ($240) while Sarah contributes 20% ($60). Her complete out-of-pocket expense totals $110. When Sarah needs another filling in October priced at $150, she won't face the deductible again. She only pays her 20% coinsurance share ($30) since she already cleared her annual deductible threshold back in March.
Now picture a family situation: The Martinez household carries coverage with a $50 individual deductible and $150 family maximum. In February, their son requires a filling ($200), triggering his $50 deductible payment. Come April, their daughter needs an extraction ($250), adding another $50 toward the family's combined total, bringing them to $100. When their father requires a crown in June ($1,200), his first $50 payment completes the $150 family deductible. At that moment, everyone in the household stops paying deductibles for the remainder of that calendar year—they only handle coinsurance percentages on any subsequent procedures.
Timing creates different outcomes. When you receive substantial dental treatment early in January or February, you'll satisfy your deductible quickly and then enjoy coinsurance-only pricing for any procedures you need during the remaining ten months. If your dental needs stay limited to preventive cleanings throughout the year, you might never engage with your deductible at all, and any unused deductible amount simply disappears when the calendar flips to the new year.
Author: Olivia Davenport;
Source: ladylesliebelize.com
What Is a Good Deductible Amount for Dental Insurance
Deductibles in dental insurance policies generally fall between $0 and $150 per person each year. The amounts you'll encounter most frequently are $25, $50, $75, and $100. Unlike health insurance for medical care, where deductibles can climb into thousands of dollars, dental deductibles stay relatively modest because annual maximum benefits (typically $1,000 to $2,000) establish a ceiling on how much your insurer will pay in a year regardless of your expenses.
Identifying what counts as a good deductible for dental insurance depends on multiple considerations:
Your dental treatment history: If your mouth tends to develop cavities, you battle periodontal disease, or you're in the middle of ongoing restorative treatment, you'll probably satisfy any deductible early each year. A moderately higher deductible combined with a reduced monthly premium could actually save you money when you calculate total annual costs. On the flip side, if your dental appointments rarely involve anything beyond your six-month cleanings, your deductible level becomes almost irrelevant since preventive care sidesteps the deductible completely.
Your financial cushion: Can you comfortably handle a $100 surprise expense if you discover you need an unexpected filling? When that sum would create budget stress, a lower deductible provides more predictable cost patterns, even though you'll see your monthly premium tick upward slightly.
Premium cost relationships: Policies offering $0 deductibles frequently carry monthly premiums that run $5 to $15 higher compared to plans charging $50 or $100 deductibles. Do the annual arithmetic. When a zero-deductible plan increases your premiums by $120 over twelve months, but you usually require roughly $300 in basic dental procedures yearly, the numbers might justify paying the higher premium. But if you only occasionally need a filling every couple of years, you're essentially prepaying for coverage you rarely activate.
Household size: Bigger families face increased probability that at least one person will require dental work beyond routine cleanings. A moderate per-person deductible paired with a sensible family aggregate maximum frequently delivers the optimal balance.
A practical guideline: for individuals experiencing typical dental health who need one or perhaps two fillings every few years, a $50 deductible hits a reasonable middle ground between manageable premium costs and tolerable out-of-pocket expenses. Those blessed with excellent dental health might select higher deductibles to minimize their premium spending. People managing ongoing dental challenges should emphasize plans offering thorough coverage and reduced cost-sharing, even when the deductible sits somewhat higher.
Dental insurance is one of the most misunderstood benefits. Most people don't realize that preventive care is fully covered, and they delay visits thinking they'll have to pay out of pocket first. Understanding your deductible is the first step to using your benefits wisely
— Dr. Chad Wagener
Dental Insurance Plans With No Deductible
Dental insurance no deductible plans definitely exist in the marketplace, though you'll find them less frequently than policies carrying modest deductible amounts. These plans eliminate the upfront payment threshold, meaning your coinsurance percentage starts immediately for both basic and major treatment categories.
Benefits: The main advantage comes from cost predictability. You know precisely what percentage you'll pay for any procedure without needing to monitor whether you've crossed a threshold yet. For people requiring frequent dental interventions, this arrangement simplifies financial planning. Additionally, when you need an expensive procedure in January or February, you sidestep the initial out-of-pocket barrier.
Drawbacks: Policies without deductibles consistently charge elevated monthly premiums—sometimes $10 to $20 more each month compared to similar policies carrying $50 deductibles. Across twelve months, that premium difference accumulates to $120 through $240 in additional spending. When you only require a single filling ($200) during the entire year, you could end up paying more in extra premiums than you saved by avoiding a $50 deductible.
Ideal candidates: These policies suit individuals managing chronic dental conditions requiring multiple treatments annually, or those who strongly value predictable expenses over potential savings. They also attract people experiencing dental anxiety who might postpone necessary care if confronted with an upfront deductible payment.
Financial comparison: Imagine two hypothetical policies. Policy A carries $0 deductible, charges $45 monthly, and provides 80% coinsurance for basic procedures. Policy B requires a $50 deductible, costs $35 monthly, and also provides 80% coinsurance. Over twelve months, Policy A totals $540 in premiums; Policy B comes to $420. When you need a $200 filling, Policy A costs you $40 in coinsurance (20% of $200). Policy B costs $50 for the deductible plus $30 coinsurance (20% of the remaining $150), totaling $80. Your complete annual spending with Policy A reaches $580. With Policy B you pay $500. In this scenario, Policy B saves $80 despite carrying a deductible.
The math shifts when multiple procedures enter the picture. Two fillings totaling $400 under Policy A cost $80 in coinsurance plus $540 in premiums (combined $620). Under Policy B, you satisfy the $50 deductible one time, then contribute 20% of the remaining $350 ($70), plus $420 in premiums (combined $540). Now Policy B delivers $80 in savings.
Zero-deductible policies aren't automatically superior or inferior—they redistribute costs from point-of-service payments to monthly premium charges. Your choice should mirror your dental health patterns and financial priorities.

Author: Olivia Davenport;
Source: ladylesliebelize.com
Common Deductible Mistakes and How to Avoid Them
Mistake #1: Believing the deductible applies to every service
Plenty of people postpone their routine cleanings, incorrectly thinking they must satisfy the deductible first. Preventive care nearly universally escapes deductible requirements. Schedule your regular cleanings without hesitation—insurance typically covers them completely.
Mistake #2: Losing track of deductible progress
When you change dental offices mid-year or visit specialists in addition to your general dentist, you can lose sight of whether you've already satisfied your deductible. Obtain an Explanation of Benefits statement after every visit or log into your insurance company's member portal. Understanding your current status helps you forecast costs for treatments you're scheduling.
Mistake #3: Automatically selecting the smallest deductible
A $0 or $25 deductible appears attractive at first glance, but when it increases your monthly premium by $15 and you rarely receive dental treatment beyond cleanings, you're spending $180 every year to avoid an expense you'd never actually encounter. Compare total yearly costs—premiums plus anticipated out-of-pocket spending—rather than fixating exclusively on the deductible number.
Mistake #4: Overlooking the annual reset
When you require major dental work, calendar timing matters substantially. A crown placed in late December means you'll satisfy your deductible with mere weeks remaining in the benefit year. When circumstances allow, schedule expensive procedures in January or February so that any additional treatments during that year benefit from your already-satisfied deductible. That said, never delay necessary dental care purely for timing reasons—untreated oral health problems deteriorate and generate more expensive complications.
Mistake #5: Mixing up deductibles with annual maximums
Your deductible represents what you pay before coverage activates. Your annual maximum represents the most your plan will pay during one year. After you reach the maximum (frequently $1,000 to $1,500), you personally pay 100% of any additional treatment costs. These are distinct limits operating in opposite directions on your behalf.
Mistake #6: Ignoring family deductible provisions
Certain policies waive individual deductible requirements once the household reaches its family threshold. When your family needs extensive dental work, strategic care coordination makes financial sense. Having multiple family members approach their individual deductibles around the same time can trigger the family maximum sooner, creating immediate benefits for everyone in the household.
Comparing Dental Deductible Options
Examining how various deductible amounts affect your complete annual costs enables more informed coverage decisions. The comparison below demonstrates three typical scenarios:
| Deductible Amount | Yearly Premium Cost | Preventive Care Expense (2 cleanings, 1 checkup) | Basic Work Expense (1 filling, $200) | Major Work Expense (1 crown, $1,200) | Recommended For |
| $0 | $540 | $0 (covered completely) | $40 (20% coinsurance only) | $240 (20% coinsurance only) | Regular dental procedures needed; predictable costs preferred; comfortable with higher monthly payments |
| $50 | $420 | $0 (covered completely) | $90 ($50 deductible plus 20% of $150) | $290 ($50 deductible plus 20% of $1,150) | Typical dental health; occasional fillings required; seeking balanced cost structure |
| $100 | $360 | $0 (covered completely) | $120 ($100 deductible plus 20% of $100) | $320 ($100 deductible plus 20% of $1,100) | Exceptional dental health; rarely need beyond routine maintenance; prioritize lowest premiums |
This comparison assumes 80% coinsurance applies to basic and major categories after satisfying the deductible, and 100% coverage for prevention with zero deductible required. Your actual expenses will vary based on your specific policy, dental provider, and regional pricing.
Notice how total yearly spending shifts according to your treatment needs. Someone requiring only preventive maintenance pays exclusively their premium, making the $100 deductible plan most economical at $360 annually. Add one filling to the picture, and the $100 deductible plan costs $480 in total ($360 premium plus $120 procedure cost), while the $50 deductible plan costs $510 ($420 plus $90), and the zero-deductible plan reaches $580 ($540 plus $40). The spending gap narrows as procedure expenses climb, but the premium cost differential remains constant throughout the year.

Author: Olivia Davenport;
Source: ladylesliebelize.com
Frequently Asked Questions About Dental Insurance Deductibles
Selecting the appropriate dental insurance deductible requires balancing your oral health patterns, financial circumstances, and comfort level with risk. A deductible isn't inherently beneficial or detrimental—it's a mechanism for distributing expenses between consistent monthly premiums and treatment-time payments.
Begin by examining your dental history across the previous three years. Calculate how many fillings, extractions, or other treatments beyond cleanings you've required. If you average two or more basic procedures each year, prioritize policies offering comprehensive benefits and favorable coinsurance percentages over obsessing about deductible amounts. The deductible becomes a minor consideration when you're regularly utilizing your coverage.
If your oral health remains excellent and you seldom need treatment, explore policies carrying higher deductibles paired with reduced premiums. You'll probably never pay the deductible anyway, so why spend extra monthly for protection you won't activate? Channel those premium savings toward building emergency reserves or addressing other financial priorities.
Calculate complete annual expenses before finalizing your decision. Multiply your monthly premium by twelve, then add estimated out-of-pocket costs based on your typical dental requirements. Run this calculation across plans offering different deductible levels. The policy with the lowest deductible frequently isn't the most economical option when you factor in premium cost differences.
Remember that dental insurance functions distinctly from medical coverage. Annual benefit maximums cap your insurance payments regardless of your deductible level, and most dental expenses remain relatively foreseeable. Unlike medical emergencies that can generate devastating financial costs, dental procedures rarely surpass several thousand dollars annually. This characteristic makes dental insurance function more as a budgeting tool for anticipated care rather than protection against financial catastrophe.
Reassess your coverage each year when your benefits election period arrives. Your dental requirements evolve as you get older, and available plan options change regularly. The coverage that served you well previously might not represent your optimal choice currently. Stay educated about your benefits, monitor your deductible status as the year progresses, and ask questions whenever you need clarification from your human resources department or insurance representative.
The appropriate deductible level supports your dental health maintenance without creating financial strain. By understanding how deductibles integrate with your complete coverage package, you can make confident selections that align with both your oral health requirements and your financial objectives.
Related Stories
Read more
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.