A dentist in blue gloves holding a white ceramic dental crown with dental tools and a tooth impression on a sterile tray in a modern dental office
Dental Insurance for Crowns Guide
When your dentist mentions you need a crown, the first question that probably crosses your mind is "What will this cost me?" Individual crowns carry price tags that range dramatically—you might pay under $1,000 or over $3,000 for the same tooth, depending on where you live and what coverage you carry. Understanding insurance specifics before you schedule that procedure can save you hundreds or even thousands of dollars.
Most patients only start researching crown coverage after they've already been told they need one. At that point, your options shrink considerably. Waiting periods, annual benefit caps, and policy exclusions all work against you when you're making reactive decisions instead of proactive ones. This guide explains everything you need to know about securing coverage before that emergency appointment.
Do Dental Crowns Qualify for Insurance Coverage?
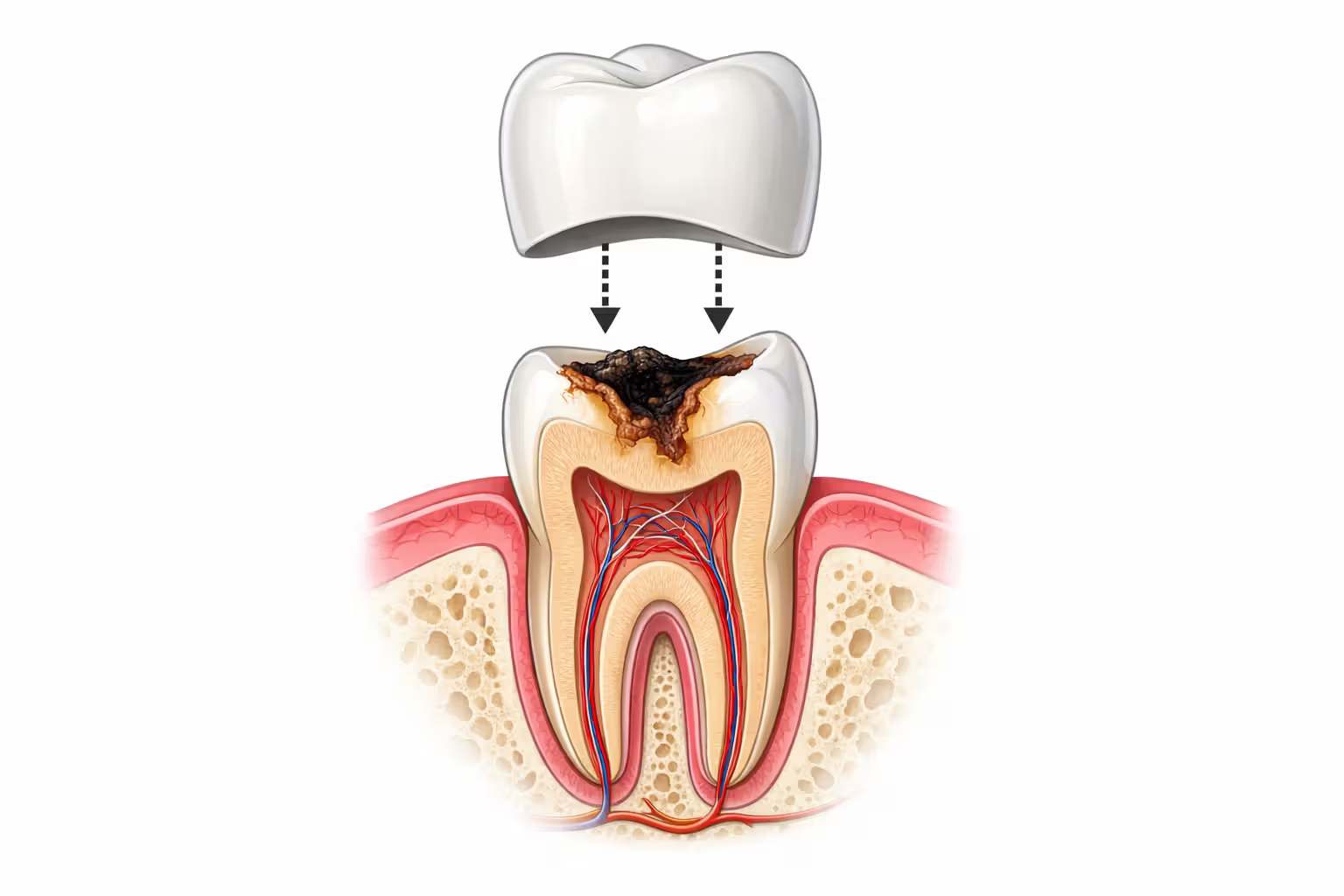
Dentists use crowns—custom-fitted caps that encase damaged teeth—to address several clinical problems. You might need one because decay has destroyed too much tooth structure for a filling to work, because an existing restoration has failed, because fractures compromise the tooth's integrity, or because root canal therapy has left the tooth vulnerable to breaking.
Insurance carriers place crowns in the "major restorative" category alongside bridges, full dentures, and implant work. This classification directly impacts both your reimbursement percentage and how long you'll wait before coverage activates.
Are dental crowns covered by insurance? The answer is usually yes, with important caveats. Traditional dental plans will pay for crowns when your dentist can document that the procedure prevents additional tooth damage or restores normal chewing function. Your dentist's notes need to show clear clinical necessity—X-rays revealing extensive decay, documentation of cracks, evidence that the tooth cannot be saved with simpler treatment.
Author: Ashley Whitford;
Source: ladylesliebelize.com
Plans reject claims when they determine the procedure serves purely aesthetic goals. Choosing to cap a front tooth that's slightly yellowed but structurally sound won't qualify. Upgrading a back tooth that functions fine just to change its appearance won't either. This distinction between necessary and elective can feel arbitrary, which is why requesting pre-approval before treatment protects you from unexpected denials.
Another common limitation: most policies won't pay for replacement crowns that fail within five to eight years unless you can prove the failure resulted from accidental trauma—injuries from falls, sports impacts, or manufacturing defects rather than normal wear. This restriction catches people off-guard, especially those who clench or grind their teeth and wear through restorations faster than average.
How Dental Insurance Plans Cover Crowns
Understanding exactly how your policy calculates benefits helps you anticipate real costs instead of facing sticker shock at the dental office.
Percentage Coverage and Annual Maximums
Dental insurance that covers crowns typically uses the standard three-tier reimbursement model. Your plan pays 100% for diagnostic and preventive services like exams and cleanings, drops to 80% for basic work like fillings and simple extractions, then falls to 50% for major procedures including crown work.
The 50% reimbursement seems simple enough until annual benefit caps enter the picture. Standard individual plans limit total payouts to between $1,500 and $2,000 per year. Consider this scenario: your crown procedure costs $1,800 and your policy covers half—that's $900 from insurance. Sounds manageable. But if you've already submitted claims totaling $800 for other dental work this year, only $700 of your $1,500 cap remains available. Insurance pays $700, leaving you with an $1,100 bill instead of the $900 you expected.
Group plans through employers sometimes offer more generous annual caps—$2,500 to $3,000 are common, and a small percentage of premium plans eliminate annual maximums entirely. These higher-limit plans usually come with steeper monthly costs, but the extra coverage becomes invaluable if you need extensive dental work.
Fee schedules add another layer of complexity. Insurance companies negotiate contracted rates with dentists in their networks. When your dentist bills $1,600 for a crown but your policy's fee schedule shows $1,200 as the "usual and customary rate" for that procedure in your area, the insurer bases its 50% calculation on $1,200, not the actual charge. They send $600 to your dentist. You're responsible for the $600 coinsurance plus the $400 difference between actual and allowed charges—$1,000 total instead of $800.

Author: Ashley Whitford;
Source: ladylesliebelize.com
Waiting Periods Explained
What dental insurance covers crowns the moment you enroll? Very few individual market plans. The vast majority impose mandatory delays—typically six to twelve months—before they'll pay benefits for major dental work.
Why do these waiting periods exist? Insurance companies want to discourage "adverse selection," the practice of enrolling only when you know you need expensive treatment, then canceling after the bill is paid. From a business standpoint, this protects the risk pool from unsustainable losses. From your perspective, it means you need to think ahead.
Standard waiting period frameworks look like this: - Preventive services (cleanings, fluoride, exams): immediate coverage - Basic restorative work (fillings, basic extractions): three to six month delay - Major procedures (crowns, root canals, bridges): six to twelve month delay
You might escape waiting periods by proving continuous prior coverage. When you're switching carriers without any gap in coverage, some insurers will credit your time under the previous plan. This isn't automatic—you'll need to provide documentation and ask specifically about crediting provisions during enrollment.
Finding Dental Insurance That Covers Crowns Immediately
Dental insurance that covers crowns with no waiting period does exist, though you'll access it primarily through specific enrollment channels.
Group coverage through your employer rarely includes waiting periods when you sign up during your initial eligibility window or during annual open enrollment. New employees who enroll when first eligible typically gain immediate access to full benefits, including major restorative coverage. This path represents your best bet for avoiding delays.
Individual plans marketed as "no waiting period" coverage require careful scrutiny. Many eliminate waits only for preventive and basic services while maintaining the standard six-to-twelve-month delay for major work. Truly comprehensive no-wait policies do exist in the individual market, but expect monthly premiums that run 40-60% higher than comparable plans with standard waiting periods.
Discount dental programs offer a different approach entirely. These aren't insurance—they're membership programs that negotiate reduced fees with participating providers. You pay the discounted rate in full out-of-pocket, but you avoid waiting periods, annual benefit limits, and claims paperwork. For someone who needs crown work soon but lacks coverage, a discount program charging $15-25 monthly might reduce an $1,800 crown to around $1,200—potentially better economics than paying standard fees while waiting out an insurance delay.
When evaluating plan documents, examine these specific elements: - Precise waiting period language under "major restorative care" or "prosthodontic services" - Whether delays apply to all enrollees or only to new customers without provable prior coverage - Whether the carrier offers a buy-up option that reduces or eliminates waiting periods for an additional fee
The most common mistake I see is patients assuming their new policy covers everything right away. I recommend enrolling in dental coverage while your teeth are healthy, not after you're told you need major work. Those mandatory waiting periods are enforced strictly, and attempting to rush treatment before your coverage activates often results in compromised outcomes.
— Dr. Sarah Mitchell
Cost of Dental Crowns With and Without Insurance
What you actually pay for crown work depends on multiple variables: the material your dentist selects, regional price variations, and whether your provider participates in your insurance network.
How much are dental crowns with insurance? After your policy's 50% reimbursement, expect personal responsibility ranging from $400 to $1,500 per tooth, varying by crown type and your dentist's standard fees. The cost of dental crowns without insurance spans from approximately $800 to $3,000 for each tooth.
Material choice drives significant cost variation. Porcelain-fused-to-metal crowns combine strength with acceptable aesthetics at mid-range pricing. All-ceramic or all-porcelain options deliver superior appearance for visible front teeth but command premium pricing. Gold and other metal alloy crowns offer maximum longevity and require minimal tooth reduction, though the visible metal makes them unpopular for cosmetic zones. Zirconia crowns blend exceptional strength with natural appearance but sit at the highest end of the price spectrum.
Where you live influences pricing more than most people expect. Identical crown procedures might cost $900 in rural Arkansas versus $2,500 in San Francisco. Insurance fee schedules attempt to account for these regional cost differences, but significant gaps between actual dentist charges and reimbursed amounts still occur frequently.
| Crown Material | Full Fee Without Coverage | Insurance Contribution (50% coinsurance) | Your Expected Responsibility |
| Porcelain-Fused-to-Metal | $1,100 - $1,600 | $550 - $800 | $550 - $800 |
| All-Ceramic/All-Porcelain | $1,200 - $2,000 | $600 - $1,000 | $600 - $1,000 |
| Gold/Metal Alloy | $1,300 - $2,100 | $650 - $1,050 | $650 - $1,050 |
| Zirconia | $1,500 - $2,500 | $750 - $1,250 | $750 - $1,250 |
| Temporary Crown | $300 - $600 | $150 - $300 | $150 - $300 |
These estimates assume your dentist's charges align reasonably with your insurance company's fee schedule and that you haven't yet reached your annual benefit maximum. Actual out-of-pocket amounts can vary substantially.
Auxiliary expenses often surprise patients. Crown procedures typically span two separate appointments—the first for tooth preparation and temporary crown placement, the second for permanent crown delivery and cementation. Some policies reimburse temporary crowns separately from the permanent restoration, while others bundle everything into a single fee. Laboratory fabrication costs, local anesthesia, and core buildup materials might appear as distinct charges on your statement.
When your tooth requires a post-and-core foundation before the crown can be placed (common after endodontic treatment), that's an additional $250-$600. Your insurance might process this as a separate covered service, or they might deny it claiming the fee should be included in the crown charge—another reason why pre-authorization prevents billing disputes.
Plans That Cover Root Canals and Crowns Together
Root canal therapy and crown placement frequently occur in sequence. Endodontic treatment removes infected pulp tissue from inside your tooth, eliminating pain and infection. However, the access cavity and removal of internal tooth structure significantly weakens what remains. A protective crown then reinforces and seals the treated tooth.
Dental insurance that covers root canals and crowns immediately is uncommon since both procedures fall under major restorative care subject to identical waiting periods. Nevertheless, the timing of how you submit claims can substantially affect your coverage.
Author: Ashley Whitford;
Source: ladylesliebelize.com
Strategic patients sometimes space these related procedures across calendar years to maximize available benefits. Imagine your root canal in November costs $1,200 with your plan covering $600 (50% coinsurance). You've now consumed $600 of your $1,500 annual maximum, leaving $900 remaining. If you schedule the crown placement in January, your annual maximum resets completely, providing another $750-$1,000 in available coverage rather than just the $900 remnant from the previous year.
This approach only works when your tooth can safely wait for the crown. Dentists routinely place temporary crowns or substantial fillings after root canal completion, protecting the tooth for several weeks or a few months. Delaying too long risks tooth fracture or recontamination of the canal system. Never postpone clinically necessary treatment just to optimize insurance timing—ask your dentist how long you can safely wait without compromising the tooth.
Insurance carriers sometimes bundle root canal and crown claims when you submit them simultaneously, applying your annual maximum to the combined charges. Other times they process them as distinct unrelated procedures. This difference significantly affects how much coverage you receive, especially when you're approaching your annual limit.
Requesting prior authorization before beginning treatment clarifies exactly what your policy will pay and allows accurate budgeting. Most insurance companies provide pre-treatment estimates within five to ten business days of receiving your dentist's proposed treatment plan.
How to Choose the Right Dental Insurance for Crown Coverage
Will dental insurance cover crowns when you actually need them? That depends on selecting a plan that matches both your oral health outlook and your financial constraints.
Begin by assessing your personal crown risk factors. Multiple older amalgam fillings, documented bruxism (teeth grinding), existing tooth fractures, or teeth with visibly large restorations all increase your likelihood of needing crown work. If you fit this profile, comprehensive major restorative coverage with generous annual maximums justifies higher premiums.
Scrutinize waiting period provisions carefully. When you're purchasing individual coverage and your dentist hasn't flagged any urgent needs, a policy with a twelve-month major services delay might work fine. Conversely, if your dentist has already identified a tooth that will need a crown within the year, you need either no-wait coverage (expensive) or a discount plan alternative.

Author: Ashley Whitford;
Source: ladylesliebelize.com
Annual maximum amounts matter more than monthly premium costs for people anticipating significant dental work. Compare these scenarios: Plan A charges $60 monthly with a $2,000 annual maximum ($720 in annual premiums), while Plan B charges $35 monthly with a $1,000 maximum ($420 in annual premiums). If you need a crown and two fillings during the year, Plan A might deliver substantially better value despite higher premiums. Calculate based on your expected treatment needs.
Provider network size affects both your choices and your costs. Plans with extensive provider networks give you more dentist options and better odds of finding practitioners whose fees align closely with insurance fee schedules. Restrictive networks might force you to travel farther or accept a dentist you haven't built a relationship with.
Study the exclusions and limitations sections in policy contracts. Certain plans exclude: - Crowns placed on teeth extracted after your enrollment date - Replacement crowns installed within five to eight years of the original - Crowns on specific tooth positions (wisdom teeth commonly excluded) - Particular crown materials (some policies won't reimburse for gold or zirconia)
Evaluate the premium-to-benefit ratio. When you're paying $50 monthly ($600 annually) for a policy with a $1,000 annual maximum, you're prepaying 60% of your potential benefit just in premiums. Unless you consistently utilize preventive services and need periodic basic work, you might achieve better economics with a discount plan or direct payment arrangements.
For people over 65, understand that Original Medicare provides no routine dental coverage, including crowns. Medicare Advantage plans sometimes bundle dental benefits, but coverage typically remains limited with various restrictions. Most Medicare beneficiaries need separate dental insurance or discount plans for meaningful crown coverage.
Frequently Asked Questions About Dental Insurance and Crowns
Crown coverage involves much more than simply checking whether your policy "covers" crowns. The reality encompasses understanding percentage-based coinsurance, annual benefit maximums, mandatory waiting periods, fee schedule limitations, and the crucial distinction between medically necessary and cosmetic treatment.
The single most valuable action you can take is enrolling in dental coverage while you're still healthy, not after a dental emergency. Waiting periods mean your strongest coverage position comes from forward planning, not reactive decision-making after your dentist discovers a cracked tooth.
When comparing policies, prioritize annual benefit maximums and waiting period provisions over monthly premium amounts. A plan costing $15 more per month that provides $500 additional annual coverage with no waiting period delivers superior value if you need crown work.
Always request pre-authorization before proceeding with crown placement. This simple administrative step clarifies your exact financial responsibility and eliminates billing surprises. If the projected costs don't fit your budget, discuss alternatives with your dentist—different crown materials, structured payment plans, or phased treatment spanning calendar years to maximize available benefits.
Dental insurance for crowns functions best as a planning tool rather than an emergency solution. Understanding your coverage details now prepares you for when you eventually need restorative dental work.
Related Stories
Read more
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.




