Patient and dentist discussing veneers and dental insurance in a modern dental office
Does Dental Insurance Cover Veneers?
Most people researching veneers quickly discover an uncomfortable truth: the majority of dental insurance plans won't pay a dime toward this procedure. The reason comes down to how insurers categorize veneers—almost always as cosmetic enhancements rather than medical necessities. Understanding this classification and the rare exceptions can save you from surprise bills and help you plan financially for the smile transformation you want.
How Dental Insurance Typically Classifies Veneers
Dental insurance companies divide procedures into three buckets: preventive care (cleanings, exams), basic procedures (fillings, extractions), and major procedures (crowns, bridges, dentures). Veneers typically fall into a fourth, unspoken category: cosmetic treatments that improve appearance without addressing medical problems.
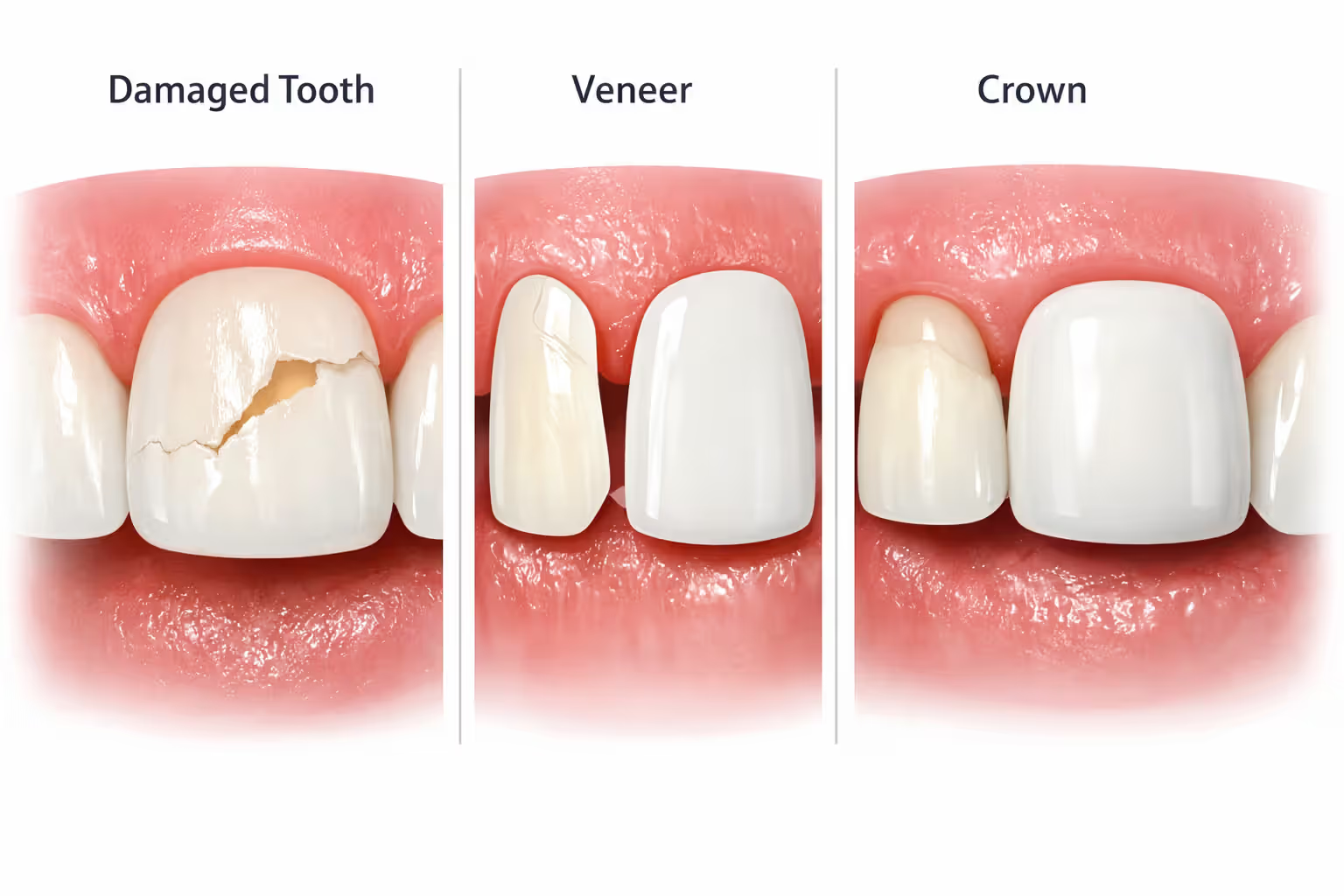
The standard insurance policy explicitly excludes coverage for procedures performed "primarily for cosmetic purposes." Since veneers—thin shells of porcelain or composite resin bonded to the front of teeth—mainly enhance aesthetics by whitening discolored teeth, closing gaps, or reshaping worn edges, insurers classify them as elective. Your plan might cover 80% of a filling or 50% of a crown, but veneers usually receive zero reimbursement.
This distinction matters because dental insurance veneers coverage depends entirely on proving medical necessity. A veneer placed to make slightly crooked teeth look straighter won't qualify. However, a veneer restoring a tooth fractured in an accident might receive partial coverage because it serves a restorative function—protecting the damaged tooth structure and preventing further decay.
The gray area emerges when a procedure accomplishes both goals. A front tooth with severe decay might need either a crown or a veneer for restoration. If your dentist recommends a veneer for structural reasons and it happens to look better than the decayed tooth, some insurers may cover a portion. Others will deny the claim, arguing a less expensive crown would suffice for medical purposes alone.
Author: Tyler Grant;
Source: ladylesliebelize.com
When Insurance May Cover Part of Veneer Costs
Specific circumstances can shift veneers from cosmetic to medically necessary, opening the door to potential insurance reimbursement. These situations require thorough documentation from your dentist explaining why veneers represent the appropriate treatment rather than an aesthetic choice.
Traumatic injury represents the clearest path to coverage. If you chip or crack a front tooth in a car accident, fall, or sports injury, the veneer restores both function and appearance. Your dentist must document the accident, often requiring incident reports or medical records. The insurer may cover the veneer at the same percentage as other major restorative work—typically 40-60% after you meet your deductible. One common mistake: waiting months after an injury to pursue treatment can raise red flags with insurers who question whether the damage truly requires immediate restoration.
Severe tooth decay or structural damage might justify veneer coverage when the tooth needs protection but retains enough healthy structure that a full crown seems excessive. Your dentist's notes must explain why a veneer provides adequate restoration. Some insurers will reimburse at crown rates if the veneer meets clinical criteria for major restorative work.
Congenital conditions affecting tooth development occasionally qualify for coverage. Enamel hypoplasia (underdeveloped enamel), amelogenesis imperfecta (genetic enamel defects), or dentinogenesis imperfecta (abnormal dentin formation) can leave teeth weak, discolored, and prone to damage. When veneers protect compromised teeth from fracture or decay, insurers sometimes classify them as medically necessary. Expect to provide genetic testing results, childhood dental records, and detailed treatment justification.
Functional bite problems rarely justify veneers alone, but when combined with orthodontic treatment or jaw surgery, veneers might receive partial coverage as part of a comprehensive treatment plan addressing malocclusion. The veneer must demonstrably improve bite function, not just appearance.
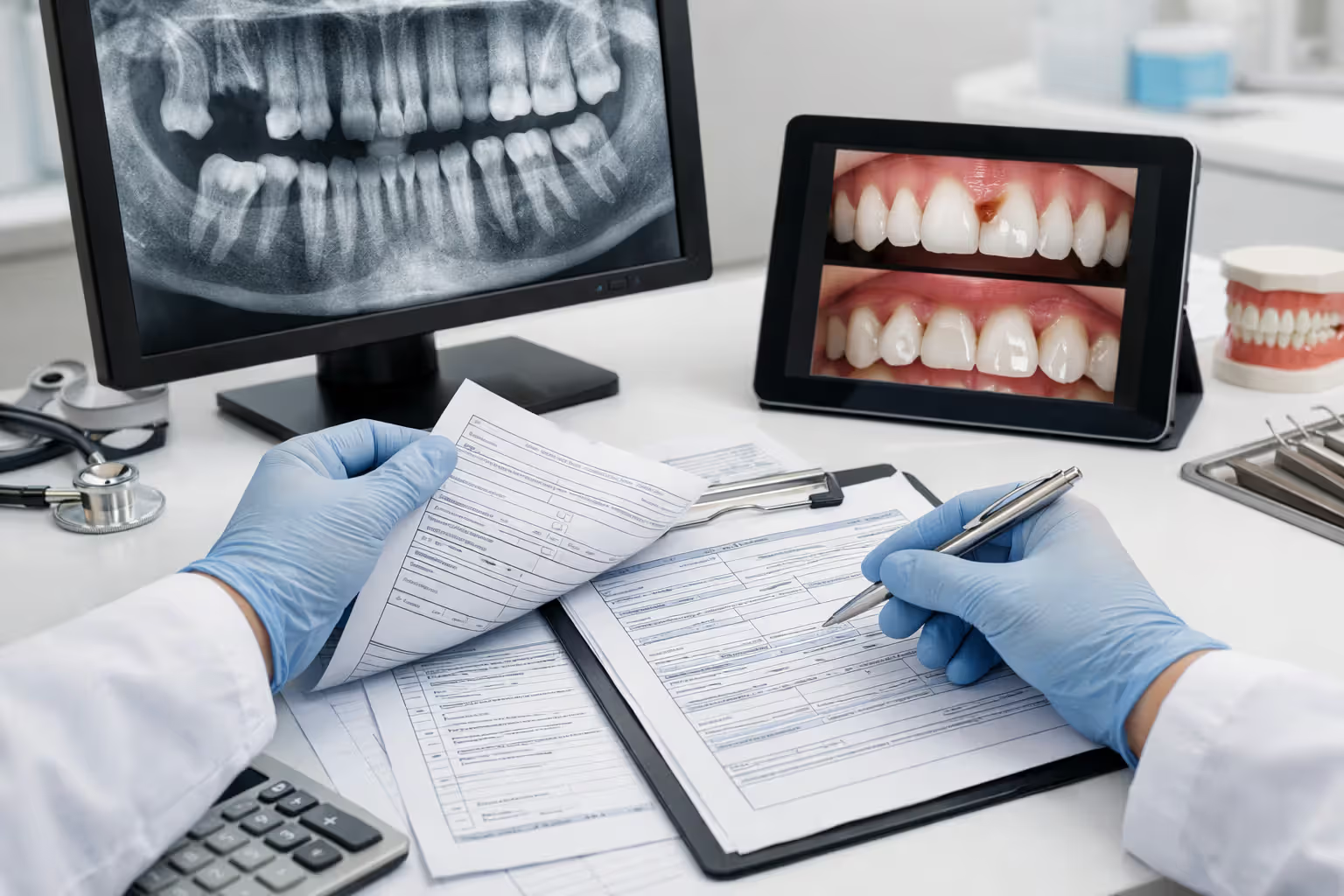
Documentation requirements cannot be overstated. Your dentist needs to submit pre-treatment X-rays, clinical photographs, a detailed narrative explaining medical necessity, and a treatment plan showing why alternatives won't work. Generic notes about "restoring tooth structure" typically get denied. Specific language about protecting pulp vitality, preventing fracture propagation, or restoring lost vertical dimension carries more weight.
Author: Tyler Grant;
Source: ladylesliebelize.com
What to Expect from Different Insurance Plan Types
Not all dental insurance operates identically. The type of plan you carry significantly affects whether you'll receive any veneer reimbursement and how much you'll pay out of pocket.
PPO Plans and Veneer Coverage
Preferred Provider Organization (PPO) plans offer the most flexibility and the best chance—however slim—of securing partial veneer coverage. PPO plans let you visit any dentist, though staying in-network reduces costs through negotiated fee schedules. When veneers qualify as medically necessary, PPO plans typically cover them at 40-50% of the allowed amount after you've met your annual deductible (usually $50-150 per person).
The catch: most PPO plans cap annual benefits at $1,500-2,000. If you need multiple veneers, you'll hit this maximum quickly. A single porcelain veneer might cost $1,200-2,500, so even with 50% coverage, you're paying $600-1,250 per tooth, and your annual maximum covers only one or two teeth. Many patients spread veneer placement across multiple calendar years to maximize insurance benefits.
PPO plans also require pre-authorization for major procedures. Your dentist submits treatment plans to the insurer, who reviews and approves, denies, or requests additional information. This process takes 2-4 weeks. Skipping pre-authorization and proceeding with treatment means you might pay 100% if the insurer later denies the claim.
HMO and Discount Dental Plans
Health Maintenance Organization (HMO) dental plans work differently. You select a primary dentist from a network and receive care only from that provider (except emergencies). HMO plans charge low monthly premiums—sometimes $10-30 per month—but offer minimal coverage for anything beyond preventive care.
Will dental insurance cover veneers under an HMO? Almost never. HMO plans explicitly exclude cosmetic procedures, and even medically necessary veneers face steep denials. The trade-off: HMO dentists sometimes offer reduced self-pay rates for veneers since you're already a plan member. You might pay $800-1,200 per veneer instead of $1,500-2,500, but you're still covering 100% of the cost.
Discount dental plans aren't insurance at all—they're membership programs offering reduced fees at participating dentists. You pay an annual membership fee ($100-200) and receive 10-60% discounts on various procedures. Veneers might be discounted 15-25%, which helps but doesn't compare to insurance reimbursement. These plans work best for people who lack employer-sponsored dental insurance and want to reduce out-of-pocket costs for elective procedures.
| Insurance Plan Type | Typical Coverage for Cosmetic Veneers | Coverage for Medically Necessary Veneers | Pre-Authorization Required | Estimated Out-of-Pocket Percentage |
| PPO Plans | 0% (excluded) | 40–50% of allowed amount | Yes, for major procedures | 50–60% after deductible |
| HMO Plans | 0% (excluded) | Rarely covered; case-by-case | Yes, often denied | 90–100% |
| Discount Plans | Not insurance; discount only | Not insurance; discount only | No (not insurance) | 75–90% with discount |
| Individual Plans | 0% (excluded) | Limited; strict medical necessity | Yes, heavily scrutinized | 80–100% |
Out-of-Pocket Costs If Insurance Doesn't Cover Veneers
When dental insurance cover veneers isn't an option—which describes most situations—you need realistic cost expectations. Porcelain veneers, the gold standard for durability and appearance, range from $1,200 to $2,500 per tooth in most U.S. markets. Coastal cities and high-cost areas push toward the upper end; smaller cities and rural areas trend lower.
Composite resin veneers cost less, typically $400-1,200 per tooth, but last only 5-7 years compared to 10-15 years for porcelain. The upfront savings disappear when you factor in replacement costs. Most cosmetic dentists recommend porcelain for front teeth that show when you smile.
A full smile transformation covering 6-8 upper front teeth runs $7,200-20,000 for porcelain veneers. Some patients add lower teeth for symmetry, pushing totals to $15,000-40,000. These figures assume healthy teeth requiring minimal prep work. Teeth with decay, old fillings, or gum disease need additional treatment first, increasing costs.
Many dental practices offer in-house financing or work with third-party lenders like CareCredit, LendingClub, or Alphaeon. These programs provide promotional periods—often 12-24 months interest-free if you pay the balance before the deadline. Miss that deadline, and deferred interest (often 20-30% APR) applies retroactively to the original balance. Read terms carefully and calculate whether you can realistically pay off the balance during the promotional period.

Author: Tyler Grant;
Source: ladylesliebelize.com
Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA) can fund veneers regardless of whether insurance covers them. Both accounts use pre-tax dollars, effectively discounting your cost by your marginal tax rate (22-37% for most professionals). If you're paying $15,000 for veneers and you're in the 24% tax bracket, using HSA/FSA funds saves $3,600. FSA funds must be used within the plan year (some plans allow small carryovers), while HSA funds roll over indefinitely.
Some patients negotiate package pricing with dentists. If you're getting 8 veneers, ask whether the per-tooth price drops for multiple units. A dentist charging $1,800 per veneer might agree to $1,500 per tooth for a full set, saving you $2,400. Cash payment sometimes yields additional discounts since the practice avoids credit card processing fees.
How to Check Your Dental Insurance Veneer Benefits
Before scheduling veneer consultations, invest time understanding your actual coverage. Assumptions lead to expensive surprises.
Start with your insurance policy documents—the Summary Plan Description (SPD) or Evidence of Coverage (EOC). These documents list covered services, exclusions, annual maximums, and coinsurance percentages. Search for "cosmetic" and "veneers" specifically. Most policies include language like "procedures performed primarily for cosmetic purposes are not covered" or list veneers under excluded services.
If your policy doesn't explicitly exclude veneers, or if you believe your situation qualifies as medically necessary, call your insurance company directly. Have your policy number, group number (if employer-sponsored), and dentist's information ready. Ask these specific questions:
- Does my plan cover veneers under any circumstances?
- What documentation proves medical necessity for veneer coverage?
- What percentage does the plan cover for medically necessary veneers?
- Does veneer coverage count toward my annual maximum?
- Do I need pre-authorization, and how long does that process take?
- Which procedure codes does the plan recognize for veneers (typically D2962 for porcelain or D2963 for resin)?
Document the call: note the representative's name, date, time, and reference number. Insurance companies sometimes provide incorrect information over the phone, and having documentation helps if you need to appeal a denied claim.
Your dentist's billing office can also verify benefits, but they're checking the same information you can access. Don't rely solely on the front desk staff saying "insurance should cover this." Request that they submit a pre-determination (also called pre-authorization or pre-treatment estimate) to your insurer. This formal process involves your dentist submitting X-rays, photos, and a treatment plan to the insurance company, which responds with a coverage determination before you proceed with treatment.

Author: Tyler Grant;
Source: ladylesliebelize.com
Pre-determinations aren't guarantees—insurers can still deny claims after treatment—but they significantly reduce surprises. If the pre-determination comes back with 0% coverage, you know exactly what you'll pay before committing to the procedure.
Are veneers covered by dental insurance in your specific case? The only way to know definitively is through this verification process. Skipping it and hoping for the best leads to claim denials and financial stress.
Alternative Coverage Options and Cost-Saving Strategies
When traditional dental insurance for veneers falls short, several alternatives can reduce your financial burden.
Many patients assume their insurance won't cover veneers and don't even ask about exceptions. When veneers restore function after trauma or address congenital defects, we've successfully secured partial coverage for about 15-20% of our patients. The key is thorough documentation showing medical necessity, not just aesthetic improvement. We photograph the damaged tooth structure, detail how the veneer protects remaining tooth material, and explain why alternative treatments won't work. It requires extra effort, but it's worth pursuing if your situation qualifies.
— Dr. Jennifer Hartman
Supplemental dental insurance offers additional coverage beyond your primary plan, but read the fine print carefully. Most supplemental plans still exclude cosmetic procedures, and those that cover veneers impose waiting periods (6-12 months before major services are covered) and lower annual maximums ($1,000-1,500). You might pay $30-60 monthly in premiums for benefits that barely offset costs. Supplemental insurance makes sense if you're planning extensive dental work over several years, but it rarely pays off for a single veneer procedure.
Dental savings plans (membership discount programs) provide immediate access to reduced fees without waiting periods. Annual memberships cost $100-200 for individuals or $150-350 for families. Participating dentists offer 10-60% discounts on procedures. Veneer discounts typically land around 15-25%, which on a $15,000 treatment saves $2,250-3,750. The math works if your savings exceed the membership fee, which they usually do for major cosmetic work.
Dental schools offer significantly reduced prices—often 30-50% less than private practices—because dental students perform procedures under licensed faculty supervision. The trade-offs: longer appointment times (students work slower and require faculty checks), less experienced practitioners, and limited appointment availability. Quality generally remains high since faculty review every step, but the experience differs from a private cosmetic practice. Major dental schools in your state likely offer veneer services; call admissions offices for information about their cosmetic dentistry programs.
Medical tourism attracts Americans seeking 50-70% savings on dental work in countries like Mexico, Costa Rica, Colombia, or Thailand. A veneer costing $1,800 in the U.S. might run $600-900 abroad. Before booking flights, research risks: varying quality standards, limited recourse if problems arise, difficulty with follow-up care, and potential language barriers. If you pursue this route, choose accredited facilities (look for American Dental Association equivalents in other countries), read extensive reviews, and factor in travel costs. Some patients combine dental work with vacation, but complications requiring return trips erase savings quickly.
Negotiating with providers works more often than people expect. Dentists set their own fees and can adjust them. If you're paying cash (not using insurance), ask for a discount. Explain you're considering multiple providers and price matters. Some dentists offer 5-10% discounts for cash payment, upfront payment, or multiple procedures. The worst they can say is no.
FAQ: Dental Insurance and Veneers
The reality check: if you're considering veneers for cosmetic reasons—brighter, straighter teeth to boost confidence—plan to pay the full cost yourself. Does insurance cover dental veneers in these situations? No. Standard dental insurance treats veneers like teeth whitening or orthodontic treatment for adults: elective procedures that improve appearance but don't address medical problems.
However, if your teeth suffered damage from accidents, disease, or congenital conditions, don't assume coverage is impossible. The verification process—reading your policy, calling your insurer, and getting pre-authorization—takes a few hours but could save thousands of dollars. Work with a dentist experienced in documenting medical necessity who understands insurance requirements.
For purely cosmetic cases, explore every cost-reduction strategy: HSA/FSA accounts for tax savings, dental savings plans for discounted fees, payment plans to spread costs over time, and dental schools for reduced rates. Compare quotes from multiple providers since veneer pricing varies significantly even within the same city.
Budget realistically for long-term maintenance. Veneers aren't lifetime solutions—porcelain lasts 10-15 years before requiring replacement, and composite lasts 5-7 years. Factor replacement costs into your financial planning. A $15,000 smile makeover becomes a $30,000 investment over 15 years when you account for eventual replacements.
The decision to get veneers shouldn't hinge solely on insurance coverage. If veneers will significantly improve your quality of life and you can afford them without financial hardship, the investment might be worthwhile even without insurance help. But enter the process with accurate expectations about costs, coverage, and long-term commitments. The worst financial mistakes happen when patients assume insurance will cover procedures without verification, then face surprise bills they can't afford.
Understanding what dental insurance covers veneers under which circumstances, knowing your specific plan's benefits, and exploring all cost-reduction options puts you in control of both the clinical and financial aspects of your dental care. That knowledge transforms an overwhelming decision into a manageable one.
Related Stories
Read more
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.