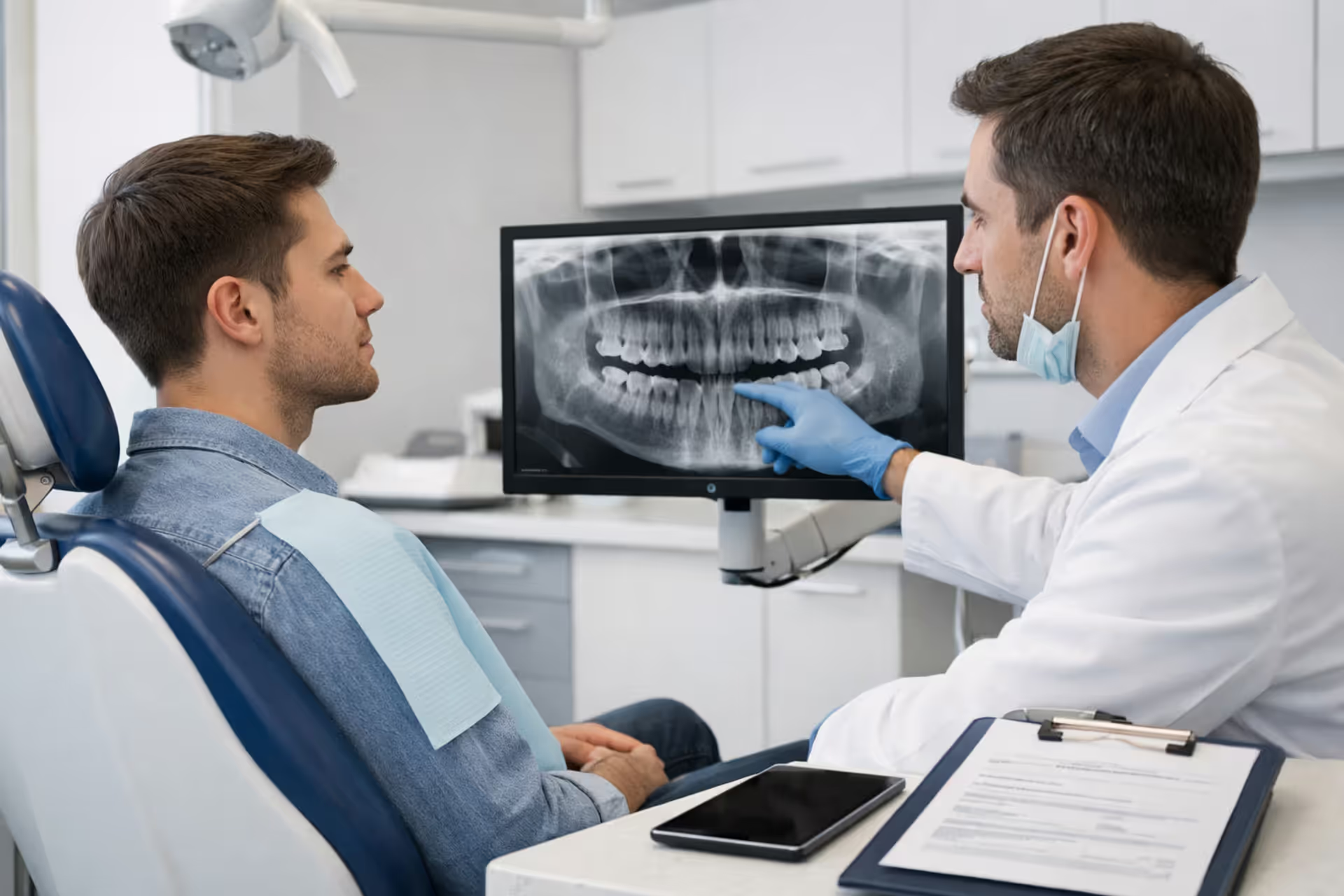
Dentist explaining wisdom teeth removal and insurance coverage to a patient
Does Dental Insurance Cover Wisdom Teeth Removal
Content
Content
Wisdom teeth removal ranks among the most common oral surgery procedures in the United States, with roughly 5 million extractions performed annually. Yet many patients discover their insurance coverage only after scheduling the procedure—sometimes leading to unexpected bills exceeding $3,000 for all four teeth.
Most dental insurance plans do cover wisdom teeth removal, but the extent of that coverage varies dramatically based on your specific plan type, the reason for extraction, and whether the procedure is deemed medically necessary. Understanding these distinctions before you sit in the oral surgeon's chair can save you hundreds or even thousands of dollars.
How Dental Insurance Typically Covers Wisdom Teeth Removal
Dental insurance wisdom teeth coverage typically falls under the "oral surgery" or "major services" category in your benefits breakdown. This classification matters because it directly determines your out-of-pocket costs.
Standard dental plans divide procedures into three tiers:
- Preventive services (cleanings, X-rays): Usually covered at 80-100%
- Basic services (fillings, simple extractions): Typically covered at 70-80%
- Major services (crowns, bridges, oral surgery): Generally covered at 50-60%
Does dental insurance cover wisdom teeth removal at the same rate as a routine filling? No. Because wisdom teeth extraction qualifies as oral surgery, most plans cover only 50% of the procedure cost after you meet your deductible. If your oral surgeon charges $400 per tooth for surgical extraction, you'll pay roughly $200 per tooth out of pocket, plus your annual deductible if you haven't met it yet.
Annual maximums create another limitation. Most dental plans cap benefits at $1,000-$2,000 per calendar year. Removing all four wisdom teeth can easily cost $1,600-$3,200 depending on complexity and your geographic location. If your plan maxes out at $1,500 annually and covers 50% of a $2,400 procedure, you'll receive only $1,200 in benefits—not the full $1,500 maximum—because your coverage percentage applies first.

Author: Olivia Davenport;
Source: ladylesliebelize.com
Does dental insurance cover wisdom teeth that haven't erupted yet? Yes, but the coverage percentage remains the same. Impacted wisdom teeth often require more complex surgical techniques, which increases the base cost even though your insurance percentage doesn't change.
Types of Dental Plans That Cover Wisdom Teeth
Not all dental insurance that covers wisdom teeth removal operates identically. The plan structure significantly affects your access to care and final costs.
PPO (Preferred Provider Organization) plans offer the most flexibility for oral surgery. You can visit any licensed oral surgeon, though staying in-network typically saves 20-40% on the procedure cost. Most PPO plans classify wisdom teeth extraction as a major service with 50% coinsurance. These plans work well if you've already established a relationship with a specific oral surgeon or need specialized care.
HMO (Health Maintenance Organization) dental plans require you to select a primary dentist from the network and obtain referrals for specialists. Dental insurance for wisdom teeth under HMO plans often involves fixed copayments rather than percentage-based coinsurance—you might pay $150-$300 per tooth regardless of the actual procedure cost. The trade-off: severely limited provider choices and potentially longer wait times for referrals.
Indemnity plans (also called traditional insurance) let you visit any provider without network restrictions. Under these plans, you'll usually handle the full payment at the appointment, then file paperwork with your carrier to receive your benefit portion back within 30-45 days. What dental insurance covers wisdom teeth removal with the fewest restrictions? Indemnity plans, though they're increasingly rare and usually more expensive in monthly premiums.
Discount dental plans aren't insurance at all—they're membership programs offering reduced fees at participating dentists. You'll pay 20-50% less than standard rates, but you're still responsible for the full discounted amount. These work best for people who need immediate wisdom teeth removal but don't have waiting periods on traditional insurance.
Dental insurance that covers wisdom teeth most comprehensively? PPO plans from major carriers typically provide the best balance of coverage, provider choice, and predictable costs for oral surgery procedures.
What Affects Your Out-of-Pocket Costs for Wisdom Teeth Removal
Even with dental insurance for wisdom teeth removal, several factors determine your final bill.
Deductibles must be satisfied before coverage kicks in. Most dental plans have deductibles between $50-$150 per person annually. If you haven't had other dental work this year, you'll pay this amount first, then your coinsurance percentage applies to the remaining cost.
Waiting periods catch many people off guard. Insurance companies frequently require you to maintain active coverage for six months to a full year before they'll pay benefits for oral surgery procedures. Enrolling in a new plan in March doesn't guarantee coverage for a wisdom tooth extraction scheduled in April. Some plans waive waiting periods if you had continuous prior coverage, but gaps longer than 63 days usually reset the clock.
In-network versus out-of-network providers create substantial cost differences. An in-network oral surgeon might charge $350 per surgical extraction, while an out-of-network provider bills $550 for the identical procedure. Your insurance still covers 50% of the "allowed amount"—which might be only $400 for out-of-network care—leaving you responsible for $150 from insurance plus the $150 balance the surgeon charges above the allowed amount.
Medical necessity versus preventive extraction affects coverage in subtle ways. Dental insurance wisdom teeth policies generally don't distinguish between symptomatic and asymptomatic teeth for coverage purposes, but they do affect timing. If your dentist recommends removing healthy wisdom teeth to prevent future problems, you'll still get 50% coverage—but you might choose to schedule the procedure strategically to maximize your annual benefits.
Complexity factors increase costs without increasing coverage percentages. Simple erupted teeth might cost $150-$250 each to extract, while fully impacted teeth requiring bone removal can reach $400-600 per tooth. Your insurance covers 50% regardless, meaning your out-of-pocket expense scales with complexity.
One often-overlooked cost factor: anesthesia. General anesthesia or IV sedation adds $250-800 to your total bill, and many dental plans don't cover sedation beyond local anesthetic. Check whether your plan includes "anesthesia for oral surgery" as a covered benefit.
Author: Olivia Davenport;
Source: ladylesliebelize.com
When Medical Insurance May Cover Wisdom Teeth Removal Instead
In certain circumstances, your medical insurance—not your dental plan—becomes the primary payer for wisdom tooth extractions. Understanding when this switch occurs can dramatically reduce your expenses.
Medical insurance may become the primary payer when wisdom teeth removal involves:
Hospital-based procedures: If your oral surgeon recommends extraction in a hospital operating room rather than an office setting—common for patients with complex medical conditions, severe anxiety, or extremely impacted teeth—your medical insurance typically covers the facility fees, anesthesia, and sometimes the surgeon's fees. Your medical deductible and out-of-pocket maximum apply instead of your dental limits.
Infection or acute symptoms: An abscessed wisdom tooth causing facial swelling, fever, or difficulty swallowing may qualify as a medical emergency rather than a dental procedure. Emergency room treatment for wisdom tooth infections falls under medical coverage, though the ER will usually prescribe antibiotics and refer you to an oral surgeon for definitive treatment.
Pathology or cysts: When imaging reveals cysts, tumors, or other pathological conditions associated with wisdom teeth, extraction often qualifies as medical treatment. Your medical insurance covers pathology testing and treatment of the underlying condition, which includes removing the affected tooth.
Trauma or fracture: Wisdom teeth broken in accidents or sports injuries typically fall under medical coverage, especially if treated within 24-48 hours of injury.
The catch: you can't usually choose which insurance to bill. The procedure's setting and documentation determine whether it's a medical or dental claim. An oral surgeon performing office-based extraction of asymptomatic wisdom teeth must bill dental insurance, even if your medical coverage would pay more.
Some patients benefit from coordination of benefits when both insurances apply. Hospital-based wisdom teeth removal might see medical insurance pay 80% after your deductible, then dental insurance covering a portion of the remaining 20%—though this requires careful billing coordination and doesn't always work as smoothly as hoped.
How to Verify Your Coverage Before the Procedure
Dental insurance for wisdom teeth removal requires proactive verification to avoid surprise bills.
Step 1: Locate your Summary of Benefits (often called an Evidence of Coverage or EOB). This document lists coverage percentages by procedure category. Look for "oral surgery," "surgical extractions," or "major services." Note your annual maximum, deductible, and any waiting periods.
Step 2: Call your insurance carrier with specific questions. Generic inquiries like "Do you cover wisdom teeth removal?" yield unhelpful "yes" answers. Instead, prepare detailed questions about your current benefit status: - What percentage applies to surgical tooth extraction under procedure code D7240? - What portion of my annual deductible have I already satisfied this calendar year? - What balance remains on my yearly benefit maximum? - Does oral surgery require advance authorization from your company before scheduling? - Can you confirm whether [specific oral surgeon's name] participates in your network?
Step 3: Request a pre-authorization or predetermination from your oral surgeon's office. They'll submit your X-rays and treatment plan to your insurance, which responds with an estimate of benefits. This isn't a guarantee of payment, but it reveals potential issues before the procedure.
Step 4: Get the estimate in writing. Phone representatives make mistakes. Request a written breakdown showing the procedure codes, allowed amounts, your coinsurance, and estimated out-of-pocket costs.

Author: Olivia Davenport;
Source: ladylesliebelize.com
Step 5: Understand claim denial reasons. Common denial causes include: - Required coverage duration not yet satisfied - Yearly benefit cap already reached through other treatments - Extraction classified as "not medically necessary" - Missing diagnostic documentation (X-rays, clinical notes) - Provider outside approved network without advance authorization
If your claim is denied, request a written explanation with the specific policy language cited. Many denials can be appealed with additional documentation from your dentist explaining medical necessity.
One practical tip: schedule wisdom teeth removal early in the calendar year if possible. This gives you the full year's maximum benefit and time to address any complications before your benefits reset.
Other Dental Procedures and Insurance Coverage
Understanding how insurance treats wisdom teeth removal provides context for coverage of other common dental concerns.
The biggest mistake patients make is assuming all dental procedures are covered equally. Wisdom teeth removal falls into that expensive middle ground—it's medically necessary enough to receive some coverage, but costly enough that insurance won't pay the full amount. I always recommend patients get a pre-authorization at least two weeks before scheduling surgery. About 30% of the time, we discover issues with waiting periods, maximums, or network status that would have blindsided the patient with a massive bill.
— Dr. Jennifer Martinez
Does dental insurance cover teeth whitening? Rarely. Insurers classify whitening as a cosmetic procedure rather than medically necessary treatment. You'll pay the full $300-$800 cost out of pocket whether you choose in-office or take-home whitening. The exception: whitening to match color after trauma-related tooth repair might receive partial coverage if documented as restoring function rather than enhancing appearance.
Will dental insurance cover teeth whitening after orthodontics? No, even though many patients want whitening to complement their new smile. Cosmetic procedures remain excluded regardless of the circumstances.
Does dental insurance cover chipped teeth? Yes, but coverage depends on the repair method. Small chips repaired with bonding (CDT code D2330) typically qualify as basic services with 70-80% coverage. Larger chips requiring crowns fall under major services at 50% coverage. Chipped front teeth affecting appearance receive the same coverage as chipped molars—insurance doesn't pay extra for aesthetic zones.
| Treatment Category | Benefit Level | Insurance Pays | Counts Toward Yearly Cap? | Patient Responsibility |
| Preventive Cleaning | Prevention | 80-100% | Usually excluded | $0-$40 |
| Cavity Filling | Basic | 70-80% | Yes | $40-$90 |
| Surgical Wisdom Tooth Extraction | Major | 50-60% | Yes | $200-$400 each tooth |
| Dental Crown | Major | 50-60% | Yes | $400-$700 |
| Professional Whitening | Cosmetic | 0% | Not applicable | $300-$800 |
| Bonding for Broken Tooth | Basic | 70-80% | Yes | $50-$100 |
Insurance companies structure benefits to encourage routine preventive care through higher coverage rates while requiring patients to share costs for expensive major treatments. Purely cosmetic work receives zero coverage since it doesn't address medical problems or functional restoration.
Frequently Asked Questions About Dental Insurance and Wisdom Teeth
Wisdom teeth removal represents a significant healthcare expense, but dental insurance substantially reduces your costs when you understand how to navigate coverage. The difference between a $400 surprise bill and a manageable $200 expected expense often comes down to asking the right questions before scheduling surgery.
Start by thoroughly reviewing your specific plan's coverage for oral surgery, including your annual maximum, deductible status, and any waiting periods. Contact your insurance carrier directly with procedure codes rather than general questions. Request pre-authorization from your oral surgeon's office to identify potential coverage issues while you still have time to address them.
Consider the timing of your procedure strategically. Scheduling early in the calendar year maximizes available benefits, while patients near their annual maximum might benefit from waiting until January when benefits reset. If you need multiple dental procedures beyond wisdom teeth removal, coordinate with your dentist to prioritize treatments within your coverage limits.
Remember that medical insurance may provide superior coverage in specific scenarios—hospital-based procedures, infections requiring emergency treatment, or pathological conditions. Ask your oral surgeon whether your situation might qualify for medical rather than dental billing.
The complexity of dental insurance shouldn't deter you from necessary oral surgery. Untreated wisdom teeth can lead to infections, cysts, damage to adjacent teeth, and chronic pain—complications that ultimately cost far more than the extraction itself. By understanding your coverage and planning accordingly, you can access needed care while minimizing financial stress.
Related Stories
Read more
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.