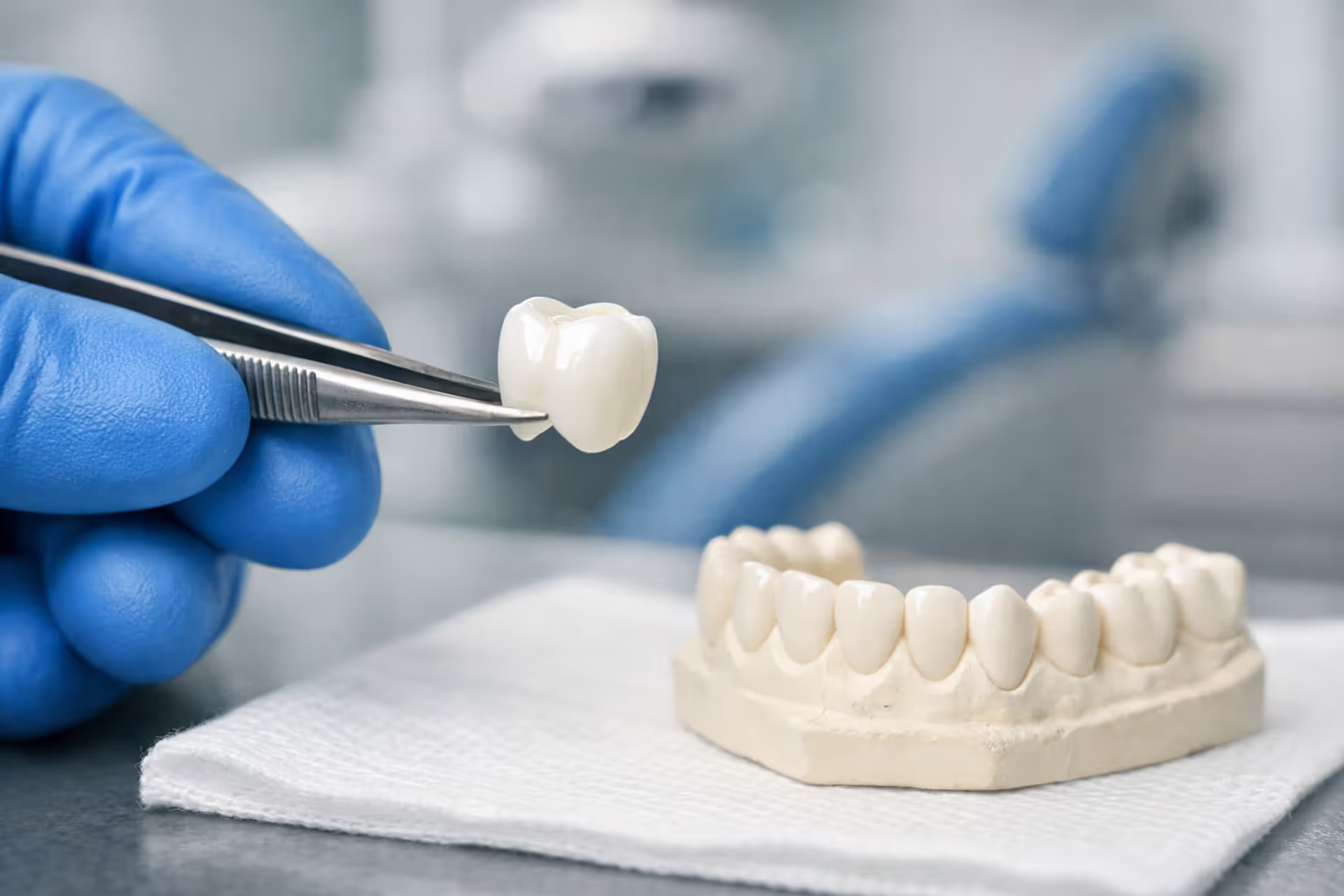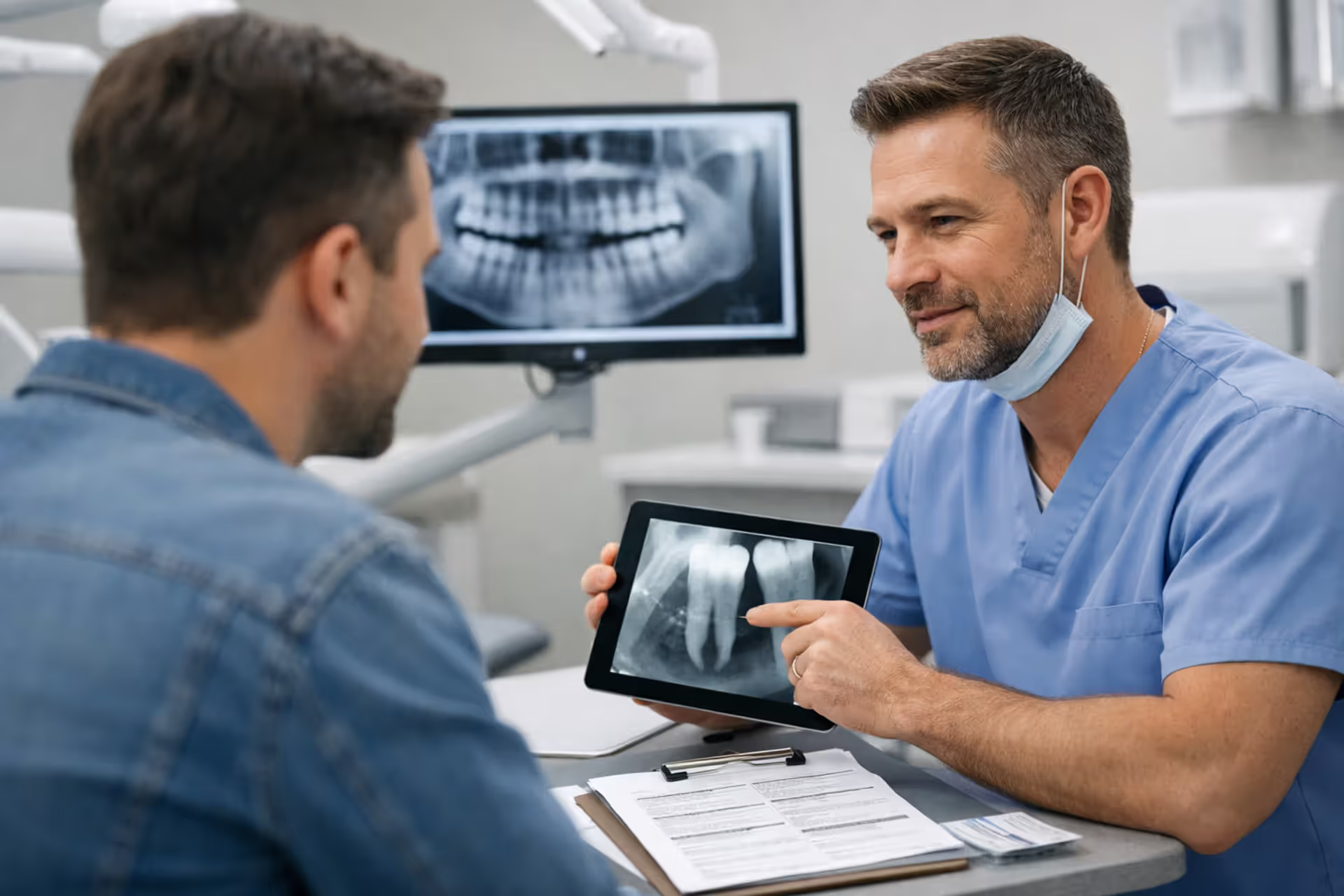
Dentist explaining dental bonding insurance options to a patient in a modern clinic
Is Dental Bonding Covered by Insurance
Here's the frustrating truth about dental bonding and insurance: whether you'll get coverage has almost nothing to do with the procedure itself. Two patients walk into the same dental office for identical bonding work—one walks out paying $80, the other pays $450. Same dentist, same technique, same tooth. The difference? How the claim gets filed and whether the insurance company believes you actually need it.
Most people discover this the hard way, sitting in the billing office after treatment. But you don't have to. Once you understand what triggers coverage approval versus denial, you can approach bonding with realistic expectations and a strategy for minimizing what you'll pay.
The real question isn't "does insurance cover bonding?" It's "does insurance cover bonding for my specific situation?"—and that answer depends on factors you have more control over than you might think.
What Is Dental Bonding and When Is It Needed
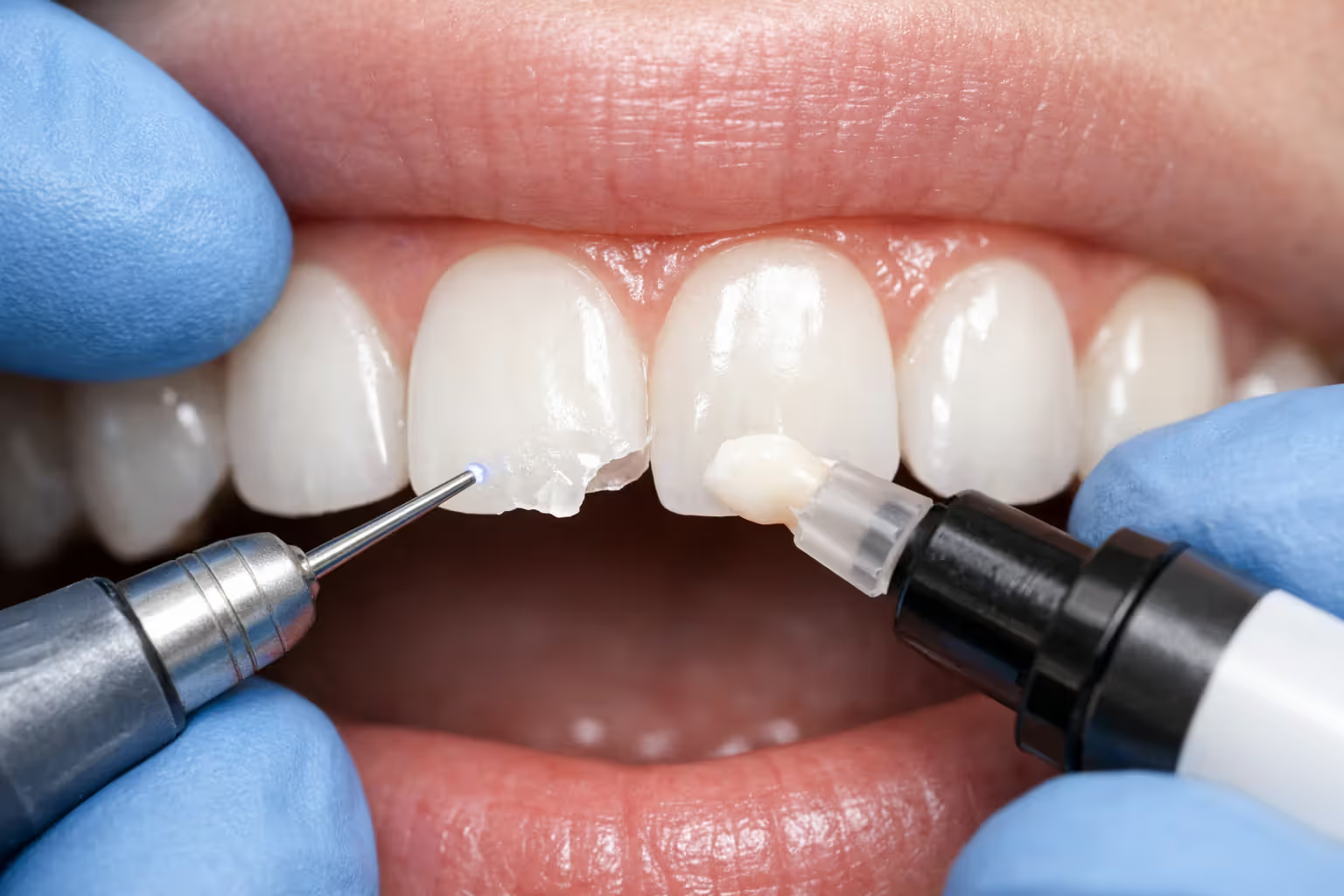
Think of bonding as sculpting with tooth-colored plastic. Your dentist roughens the tooth surface, applies a conditioning gel, then layers on composite resin—the same material used for white fillings. They shape it while it's soft, then harden it with a special UV light. Start to finish? You're looking at 30-60 minutes per tooth, and unless they're also filling a cavity, you won't need numbing.
Here's where things get complicated: bonding fixes both health problems and appearance issues. Sometimes simultaneously.
When a patient chips a front tooth biting into an apple core, bonding rebuilds the missing structure. That's restorative. When someone wants to close a small gap between perfectly healthy teeth because they don't like how it looks, bonding reshapes the teeth. That's cosmetic. Your insurance company cares deeply about this distinction. You might not even realize there is one until the claim gets denied.
Real-world scenarios blur these lines constantly. A college athlete cracks a tooth during practice—clearly needs repair. A 40-year-old with teeth stained by childhood antibiotics wants them covered—purely aesthetic. But what about exposed tooth roots from receding gums that cause pain when drinking cold water? Or a chip so small it doesn't hurt but has sharp edges that irritate your tongue? These situations fall into the gray zone where coverage becomes unpredictable.
Bonding also fills cavities when they're small and visible (front teeth where silver amalgam would show), protects sensitive root surfaces, closes gaps that trap food and increase decay risk, and repairs teeth damaged by grinding. Each scenario presents different insurance challenges depending on how the problem gets documented.
Author: Ashley Whitford;
Source: ladylesliebelize.com
How Insurance Companies Decide Bonding Coverage
Insurance carriers apply one basic filter: does this fix a health problem, or does it just make you look better? Everything flows from that question.
They'll pay to restore function or prevent disease. They won't pay to improve your appearance. Sounds simple until you realize the same bonding procedure can legitimately qualify as either one depending on the clinical details.
Let's say you chip a tooth. If that chip creates a sharp edge cutting your cheek, causes pain when chewing, or exposes the inner tooth structure to potential infection, you've got medical necessity. Document those symptoms and coverage typically goes through. But if the chip is smooth, doesn't hurt, and only bothers you when you smile? That's cosmetic—denied.
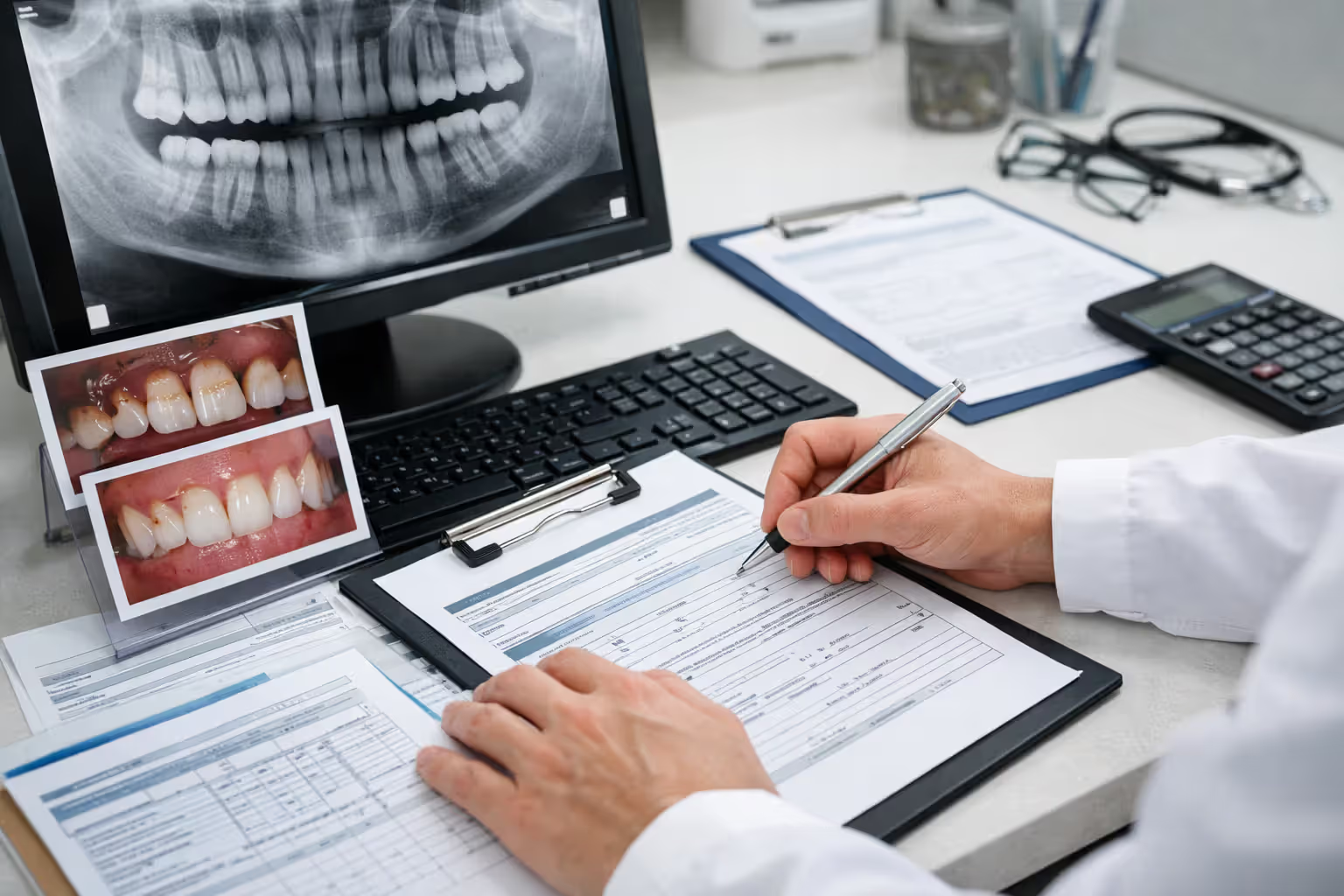
The documentation your dentist submits makes or breaks the claim. A treatment form that just lists "composite bonding, tooth #8" tells the insurance reviewer nothing about why you need it. Compare that to detailed notes: "Patient presents with 3mm fracture tooth #8, sustained falling on stairs 3 days ago. Sharp coronal edge lacerating labial mucosa. Patient reports pain when chewing on affected side. Bonding required to restore tooth contour, eliminate soft tissue trauma, and prevent pulp exposure."
Same procedure, wildly different outcomes. The second version demonstrates functional impairment with specific measurements and symptoms. It proves bonding solves a health problem, not a cosmetic preference.
Pre-authorization catches these issues before you're on the hook financially. Your dentist sends photographs, X-rays, and written justification to the insurance company, which reviews everything and issues a coverage decision. Takes two to four weeks, but you'll know exactly what you'll pay before sitting in the chair.
Author: Ashley Whitford;
Source: ladylesliebelize.com
One more critical point: some dentists are better at insurance documentation than others. A claim denial might reflect poor paperwork rather than lack of coverage. This is why getting pre-authorization matters—it forces the documentation to be thorough upfront.
| Bonding Scenario | Coverage Status | Reasoning |
| Fractured tooth from accident causing pain/sharp edges | Usually pays | Addresses functional damage; prevents additional injury and decay |
| Cavity on front tooth requiring tooth-colored filling | Usually pays | Medically necessary decay treatment; composite appropriate for visible area |
| Root exposure from gum recession with temperature sensitivity | Sometimes pays | Depends on symptom severity and recession extent documented in notes |
| Closing natural gap between front teeth (no health issue) | Usually denied | Aesthetic concern only; no disease or functional problem exists |
| Lengthening or reshaping naturally short/uneven teeth | Usually denied | Cosmetic improvement; existing teeth are healthy and work fine |
| Hiding permanent medication stains (tetracycline discoloration) | Usually denied | Appearance-only; staining creates no health risk or functional deficit |
Typical Out-of-Pocket Costs for Dental Bonding
Bonding one tooth without insurance runs $200-$600 in most places. That wide range isn't random. A dentist in Manhattan charges $500-$600 for work that costs $225 in Omaha. Same resin, same time investment, different overhead. Big cities mean higher rent, staff salaries, and operating costs—all passed to patients.
When insurance covers bonding as a basic restorative procedure (their usual classification when they cover it at all), you're looking at 70-80% coverage after your deductible. Here's the math: $400 bonding fee, 80% coverage = insurance pays $320, you pay $80. But wait—most plans have a $50 annual deductible. If you haven't used it yet, add $50 to your cost. Total out-of-pocket: $130.
Now here's the part that catches people off guard. Dental plans cap total annual benefits, typically at $1,000-$2,000. Every procedure you've had this year—cleanings, fillings, crowns, whatever—counts toward that maximum. If you've already used $1,400 of your $1,500 annual max and then need $400 worth of bonding, insurance pays the remaining $100. You're covering the other $300 yourself, regardless of coverage percentages.
Geography shifts these numbers significantly. The same insurance plan reimburses differently by region. Your policy might cover 80% everywhere, but that percentage applies to the "usual and customary rate" for your area. In rural Georgia, the usual rate for bonding might be $250. In San Francisco, it's $475. You pay 20% of whichever number applies to your zip code.
Multiple teeth don't get cheaper per tooth, though some dentists knock 10-15% off if you're bonding three or four in one session. But insurance coverage applies individually to each tooth based on medical necessity. Bond four teeth—two from an accident, two for appearance—and you'll get coverage for the accident damage only. The cosmetic work comes entirely from your pocket.

Author: Ashley Whitford;
Source: ladylesliebelize.com
Other Common Dental Procedures and Insurance Coverage
Bonding makes more sense when you see how insurance treats dental work generally. Plans divide procedures into three tiers with very different coverage levels.
Preventive Services That Insurance Usually Covers
This is where insurance actually works like you'd expect. Preventive care gets covered at 100% because preventing problems costs insurers less than fixing them later.
Routine cleanings? Covered twice a year, no deductible, nothing out of your pocket. Same for regular checkups. Periodic X-rays (bitewings yearly, full-mouth series every 3-5 years) get the same treatment. For kids, fluoride treatments and sealants typically have full coverage through age 13-14.
Emergency dental visits land in a different category despite feeling urgent. The exam might get covered at 80% as a basic service, but the actual treatment depends on what's needed. Emergency root canal? That's major work at 50% coverage. Temporary filling? Basic procedure at 70-80%. The "emergency" designation doesn't automatically mean better coverage—just faster treatment.
One question people ask constantly: will medical insurance ever cover dental work? Occasionally, yes, but only when dental treatment addresses a medical diagnosis your health plan covers. Teeth broken in a car accident might get covered under your medical policy's accident benefits. Dental work needed after oral cancer treatment sometimes qualifies as reconstructive surgery. These situations are uncommon enough that you should assume medical won't cover dental unless you get written pre-authorization.
Major Procedures with Partial or Limited Coverage
Major work is where dental insurance shows its limitations. Coverage drops to 40-50% after you've met your deductible, and annual maximums become a serious constraint.
Take implants—a single implant averages $3,000-$4,500 depending on your area. Many plans still exclude implants completely, calling them cosmetic or experimental (despite decades of proven results). Plans that do cover implants classify them as major, offering 50% coverage. So on a $3,500 implant, insurance might pay $1,750. But only if you haven't maxed out your annual benefits already.
Orthodontics (braces) for adults almost never gets coverage unless severe jaw misalignment causes pain or functional problems. For kids, some plans include orthodontic benefits—typically 50% coverage up to a lifetime maximum of $1,000-$2,000. Many basic dental plans don't include orthodontic benefits at all, so check before assuming your kid's braces will get any coverage.
Crowns, bridges, and root canals fall into major or basic categories depending on your plan. Most classify them as major (50% coverage), though some plans treat root canals as basic procedures (70-80% coverage). The variation makes it impossible to generalize—you need to check your specific plan documents.
Author: Ashley Whitford;
Source: ladylesliebelize.com
What about dental irrigation for gum disease? If your dentist performs therapeutic irrigation as part of periodontal treatment, it might get covered as disease treatment. But the portable water flossers you buy for home use? Those are out-of-pocket maintenance tools, never covered.
| Procedure | Coverage Level | Category |
| Six-month cleanings | 100% | Preventive |
| Annual exam | 100% | Preventive |
| Routine X-rays | 100% | Preventive |
| Standard fillings | 70-80% | Basic restorative |
| Bonding (when medically necessary) | 70-80% | Basic restorative |
| Crowns | 50% | Major |
| Root canals | 50-80% | Major or basic (varies by plan) |
| Dental implants | 0-50% (many exclude entirely) | Major or not covered |
| Adult braces | 0% | Cosmetic exclusion |
| Children's braces (with ortho rider) | 50% up to lifetime cap | Orthodontic |
| Emergency visit/treatment | 70-80% exam / 50-80% treatment | Basic or major |
How to Maximize Your Dental Insurance Benefits for Bonding
Getting coverage for bonding requires strategy, not luck. Start by requesting pre-authorization before scheduling anything. Your dentist submits photos, X-rays, and detailed clinical notes explaining exactly why bonding is medically necessary for your situation. The insurance company reviews everything and tells you whether they'll cover it.
This takes a few weeks, which feels annoying when you want the problem fixed now. But consider the alternative: scheduling treatment, paying your estimated portion, then getting a denial letter three weeks later saying you actually owe the full amount. Pre-authorization eliminates that scenario.

Author: Ashley Whitford;
Source: ladylesliebelize.com
If you get denied, don't just accept it. Appeal. Seriously—a shocking number of initial denials get overturned on appeal when you provide better documentation. Insurance companies deny claims liberally knowing most people won't challenge the decision. They count on it.
Your appeal should include a detailed letter from your dentist explaining medical necessity, before-and-after photos showing the problem, and specific references to your plan's coverage criteria for restorative procedures. If bonding addresses pain, difficulty chewing, soft tissue injury, or prevents further damage, spell that out explicitly. Vague claims lose appeals. Specific clinical details win them.
I see the same bonding procedure approved for one patient and denied for another every single week. The difference almost never involves the actual clinical situation—it's documentation quality. Claims that say 'patient requests bonding tooth 9' get denied. Claims that say 'bonding required to restore 4mm fracture tooth 9, patient experiencing soft tissue trauma from sharp edge, unable to chew normally without pain'—those get paid. The procedure is identical. The paperwork determines the outcome.
— Dr. Rebecca
Timing your treatment strategically can effectively double your benefits. Need bonding on multiple teeth but only some qualify as medically necessary? Schedule the covered bonding before December 31, then do the cosmetic work in January. This preserves your annual maximum for procedures insurance will pay for while letting you budget separately for the cosmetic portion.
Same logic applies to deductibles. If you've already satisfied your $50 deductible in November, schedule bonding before year-end. Wait until January and you'll pay that deductible again before coverage kicks in. Conversely, if it's early December, you haven't met your deductible, and you'll need other dental work in January anyway, waiting might make sense—let the other procedures satisfy next year's deductible.
For bonding that insurance won't cover, use your FSA or HSA if you have one. These accounts let you pay with pre-tax dollars, effectively giving you a 20-35% discount depending on your tax bracket. A 25% tax bracket means $400 cosmetic bonding paid through HSA really costs you $300 in after-tax equivalent. That's real money saved.
Frequently Asked Questions About Dental Bonding Coverage
Whether insurance covers your dental bonding depends less on the procedure itself and more on why you're getting it done. Insurers will pay for bonding that repairs damage, treats decay, or solves functional problems. They'll deny bonding performed purely for aesthetic reasons. The challenge is that many situations involve both aspects, making coverage decisions unpredictable without proper documentation.
Don't assume bonding won't be covered just because it involves appearance. If you can demonstrate a health problem—pain, difficulty eating, tissue damage, decay risk—coverage becomes possible. Pre-authorization shows you exactly what you'll pay before treatment starts, and appeals can overturn denials when you provide thorough clinical justification.
Even when insurance won't cover bonding, using HSA or FSA funds reduces your real cost through tax savings. Sometimes paying out-of-pocket for a $300 procedure that improves your quality of life makes more sense than fighting with insurance for months over an $80 reimbursement.
The larger pattern to understand: dental insurance works nothing like medical insurance. Annual maximums cap total benefits regardless of need. Procedure classifications vary wildly between carriers. Preventive care gets generous coverage specifically because it reduces insurers' long-term costs, while restorative and cosmetic work face much stricter scrutiny. Bonding occupies an awkward middle ground in this system—sometimes covered, often not, always worth investigating thoroughly before committing to treatment.
Your best defense is knowledge. Understand your specific plan's coverage categories, document medical necessity clearly, and don't hesitate to challenge denials that seem wrong. Insurance companies bet on patients accepting decisions without question. The ones who push back often get different outcomes.
Related Stories
Read more
Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.