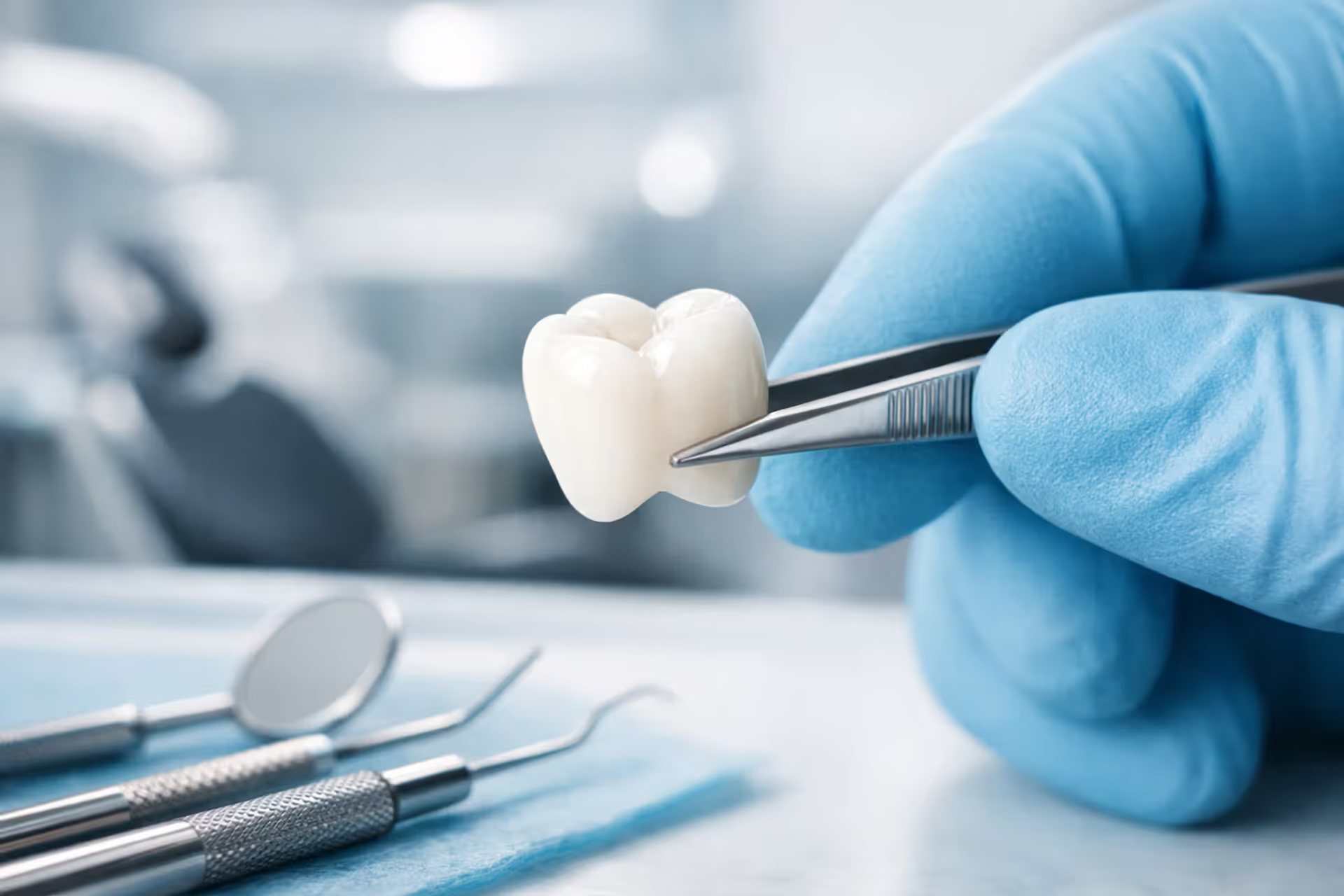
Close-up of a dentist holding a white ceramic dental crown with tweezers in a modern dental office
Are Crowns Covered by Dental Insurance?
Content
Content
Most dental insurance plans do provide coverage for crowns, but the extent of that coverage varies significantly depending on your specific policy. Understanding how your plan handles these major restorative procedures can save you hundreds or even thousands of dollars when you need crown work.
Crowns typically fall under "major services" in dental insurance classifications, which means they receive less coverage than preventive care like cleanings. Most plans cover 50% of crown costs after you meet your deductible, though you'll also need to work within annual maximum limits that many policies impose. The reality is more nuanced than a simple yes or no answer—your actual coverage depends on plan type, waiting periods, the reason you need the crown, and several other factors we'll examine in detail.
How Dental Insurance Typically Covers Crowns
Dental insurance operates on a tiered system that categorizes procedures into three main groups: preventive, basic, and major services. Crowns almost always fall into the major services category, which receives the lowest coverage percentage among the three tiers.
Preventive services—cleanings, exams, X-rays—typically receive 80-100% coverage with no deductible. Basic procedures like fillings usually get 70-80% coverage after you meet your deductible. Major services, including crowns, bridges, dentures, and root canals, generally receive only 50% coverage after the deductible.
Here's how typical coverage tiers compare:
| Coverage Tier | Coverage Percentage | Annual Maximum | Waiting Period for Major Services |
| Preventive | 100% | $1,500–$2,000 | None |
| Basic | 70–80% | $1,500–$2,000 | None or 3–6 months |
| Major (Crowns) | 50% | $1,500–$2,000 | 6–12 months |
The annual maximum is particularly important for crown coverage. If your plan has a $1,500 annual maximum and your crown costs $1,400, your insurance will pay 50%—but only up to $700. You'll pay the remaining $700 out of pocket. If you've already used $800 of your annual maximum on other procedures that year, your insurance will only contribute $700 toward the crown, even though 50% of $1,400 would normally be $700. You'd then be responsible for $1,400 minus $700, or $700.
Most plans impose waiting periods specifically for major services. You might enroll in January but need to wait until July or even the following January before crown coverage kicks in. During this waiting period, you're responsible for the full cost even though you're paying premiums.
The biggest mistake I see patients make is assuming their dental insurance works like medical insurance. Dental plans are really discount programs with strict limits. A $1,500 annual maximum hasn't changed much since the 1980s, but crown costs have tripled. Patients need to read their policy documents carefully and get pre-treatment estimates before scheduling major work
— Dr. Marcus Chen
What Affects Crown Coverage Under Your Plan
Several factors determine whether your dental insurance covers crowns and how much you'll pay out of pocket.
Medical necessity versus cosmetic reasons plays the primary role. Insurance covers crowns when they're medically necessary to restore function or protect a damaged tooth. If you broke a tooth, have severe decay, or need a crown after a root canal, coverage typically applies. However, if you want a crown purely to improve appearance on a healthy tooth, most plans exclude it as cosmetic.
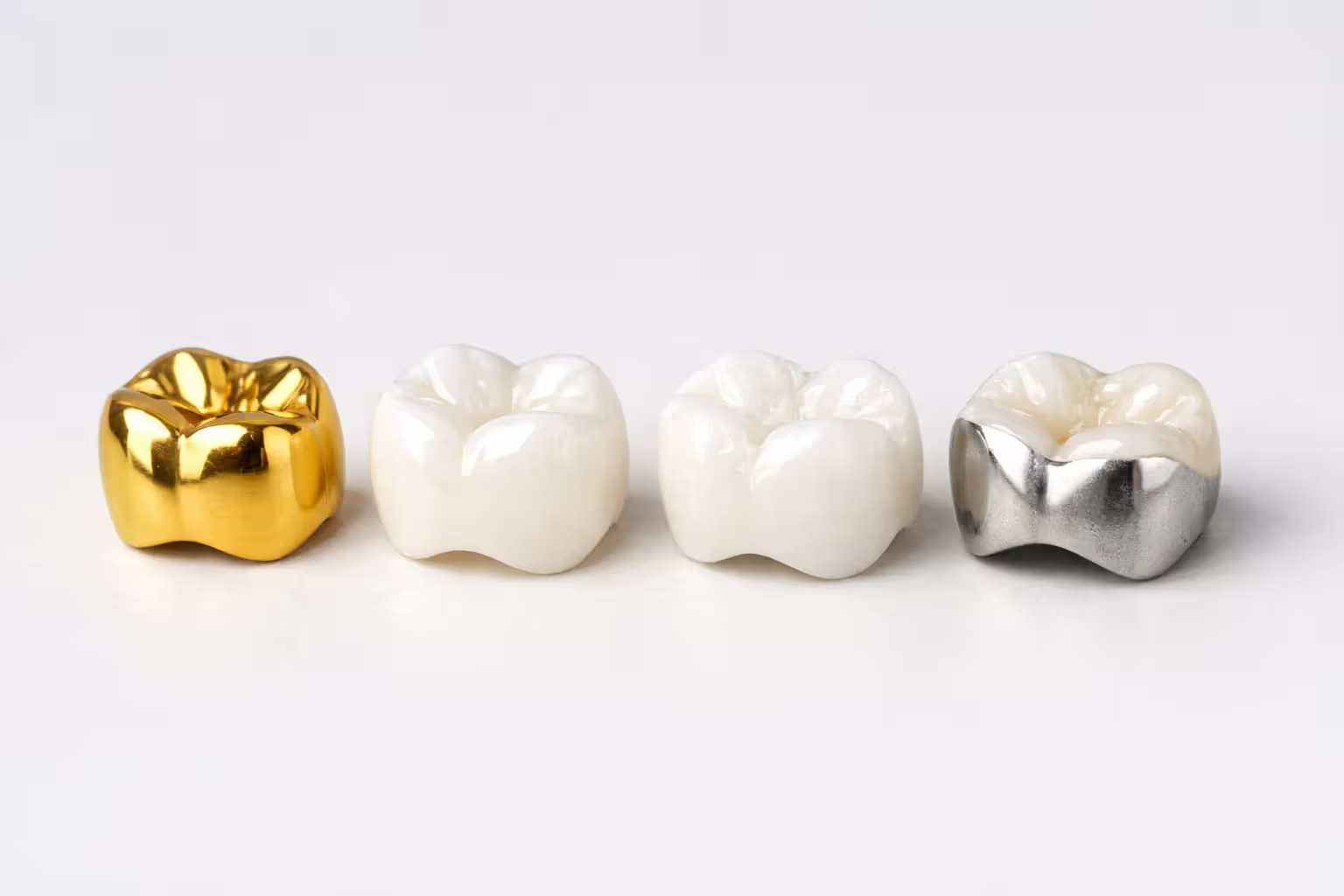
Crown material can affect coverage amounts. Porcelain and zirconia crowns cost more than metal crowns, but many plans cap reimbursement at the cost of the least expensive option that's clinically appropriate. If your dentist recommends a $1,500 zirconia crown but your plan considers a $1,000 metal crown adequate, they'll calculate your benefit based on the $1,000 amount (50% = $500), leaving you to pay $1,000 out of pocket instead of $750.
Tooth location matters for some policies. Front teeth (incisors and canines) sometimes receive better coverage for tooth-colored crowns since metal would be cosmetically unacceptable. Back teeth (molars) might have restrictions on premium materials since function matters more than appearance.
Pre-authorization requirements exist with many plans. Your dentist submits treatment details, X-rays, and justification before you schedule the procedure. The insurance company reviews everything and issues a pre-determination of benefits—essentially a coverage estimate. This isn't a guarantee, but it prevents surprises. Skipping pre-authorization can result in claim denials.
Policy exclusions vary widely. Some plans won't cover crown replacement within five years of the original crown, regardless of circumstances. Others exclude crowns on certain teeth or limit the number of crowns covered per year. Reading the fine print in your policy documents reveals these restrictions before you need the work.
Author: Daniel Mercer;
Source: ladylesliebelize.com
Dental Insurance Plans That Cover Crowns Without Waiting Periods
Finding dental insurance for crowns with no waiting period requires understanding the trade-offs involved. Plans that offer immediate major services coverage typically cost more in monthly premiums or have other limitations that offset the insurer's risk.
Employer-sponsored group plans often waive waiting periods entirely. If you enroll during your company's open enrollment period or as a new hire, major services coverage frequently begins on your effective date. This represents one of the most valuable aspects of employer dental benefits.
Some individual PPO plans advertise no waiting periods for any services, including crowns. These plans usually charge 30-50% higher monthly premiums than comparable plans with standard waiting periods. You're essentially paying upfront for the privilege of immediate access. This makes financial sense if you know you need crown work soon, but costs more over time if you remain healthy.
Discount dental plans aren't insurance but can provide immediate savings. You pay an annual membership fee (typically $100-$200) and receive 10-40% discounts on procedures at participating dentists. There's no waiting period because there's no insurance claim—you pay the discounted rate directly. For someone needing a crown immediately without insurance, this can save $200-$400.
Medicare Advantage plans with dental benefits sometimes include limited crown coverage with reduced or no waiting periods for enrollees. However, these benefits usually have low annual maximums ($1,000 or less) and may only cover crowns in specific circumstances.
The catch with no-waiting-period plans is that insurers protect themselves through other means. They might require a six-month "prior coverage" clause, meaning you must have had continuous dental insurance elsewhere before they'll waive the waiting period. Others use higher deductibles or lower annual maximums to balance their risk.

Author: Daniel Mercer;
Source: ladylesliebelize.com
Cost of Dental Crowns With and Without Insurance
Crown costs vary based on material, geographic location, and whether you're using insurance. Understanding these numbers helps you budget and evaluate whether dental insurance makes financial sense for your situation.
| Crown Material | Average Total Cost | Insurance Pays (50%) | Your Out-of-Pocket |
| Porcelain-Fused-to-Metal | $900–$1,400 | $450–$700 | $450–$700 |
| All-Porcelain/Ceramic | $1,000–$1,800 | $500–$900 | $500–$900 |
| Gold/Metal | $1,000–$1,600 | $500–$800 | $500–$800 |
| Zirconia | $1,200–$2,000 | $600–$1,000 | $600–$1,000 |
These figures assume you haven't exceeded your annual maximum and you're using an in-network provider. Out-of-network dentists typically charge 15-30% more, and your insurance may reimburse less.
Without insurance, you'll pay the full amount listed in the "Average Total Cost" column. A single crown can easily cost $1,500 or more, depending on your location. Urban areas with higher costs of living—New York, San Francisco, Boston—often see crown prices at the higher end of these ranges or even above them. Rural areas and smaller cities typically charge less.
Regional variations are substantial. A porcelain crown might cost $1,800 in Manhattan but $1,000 in rural Alabama. These differences reflect overhead costs, local competition, and regional economic factors rather than quality differences.

Author: Daniel Mercer;
Source: ladylesliebelize.com
Additional costs often accompany crown procedures. If you need a root canal before the crown, add $800-$1,500. A post and core buildup adds $200-$400. These expenses stack up quickly, making the annual maximum a real constraint for complex dental work.
Calculating whether insurance saves you money requires comparing annual premium costs against potential benefits. If you pay $50/month ($600/year) for dental insurance and need a $1,400 crown, insurance saves you $100 that year ($700 benefit minus $600 in premiums). If you need multiple crowns or other major work, the savings multiply. But if you only need preventive care, you're paying more in premiums than you receive in benefits.
Finding Dental Insurance That Covers Crowns and Implants
When you need extensive restorative work like crowns and implants, choosing the right dental insurance requires careful comparison of plan features beyond just monthly premiums.
Look at annual maximums first. A plan with a $2,000 maximum provides significantly more value for major work than one with a $1,000 cap. The difference in premiums is often only $10-$15 per month, but the extra $1,000 in coverage can be crucial when you need both a crown and an implant.
Check whether implants are covered at all. Many dental insurance plans specifically exclude implants or classify them as cosmetic. Plans that do cover implants typically treat them as major services with 50% coverage, but some exclude them entirely regardless of medical necessity. This exclusion is clearly stated in policy documents, usually in the "Limitations and Exclusions" section.
PPO plans generally offer better coverage for major restorative work than HMO or discount plans. PPOs let you see any licensed dentist, though you'll save money using in-network providers. They also tend to have higher annual maximums and more comprehensive major services coverage. HMO dental plans require you to choose a primary dentist from a limited network and often have more restrictions on major procedures.
Review the waiting period structure carefully. Some plans have a 12-month waiting period specifically for implants but only six months for crowns. Others apply the same waiting period to all major services. If you need both procedures, understanding these timelines helps you plan treatment sequencing.
Examine frequency limitations. Policies often specify how often they'll cover crown replacement (typically once every five to seven years per tooth) and may limit the number of implants covered per year or per lifetime. These restrictions significantly impact coverage if you need multiple restorations.
Get pre-treatment estimates for any major work before enrolling in a plan. Most insurers provide benefit estimates if you submit treatment plans, even before you're a member. This lets you compare exactly what different plans would pay for your specific needed procedures rather than relying on general coverage percentages.
How to Maximize Your Crown Coverage Benefits
Strategic planning can help you extract maximum value from your dental insurance when you need crown work.
Time procedures around your plan year. If you need two crowns and your annual maximum is $1,500, having one done in December and the second in January lets you use two years' worth of benefits. Each crown gets its own $1,500 maximum, potentially saving you hundreds of dollars compared to doing both in the same plan year.
Get pre-treatment estimates before scheduling any crown work. Your dentist submits the treatment plan to your insurance company, which responds with exactly what they'll cover. This eliminates surprises and gives you time to adjust your plan if the coverage is less than expected. Pre-treatment estimates typically take 2-3 weeks to process.
Use in-network providers whenever possible. In-network dentists have negotiated fees with your insurance company, often 15-30% lower than their standard rates. Your insurance calculates benefits based on these contracted fees, and you save on the difference. Out-of-network dentists can charge whatever they want, and you'll pay the difference between the insurance payment and their actual fee.
Combine FSA or HSA funds with insurance to cover your out-of-pocket costs. These tax-advantaged accounts let you pay for dental work with pre-tax dollars, effectively giving you a 20-30% discount on your portion depending on your tax bracket. If insurance covers $700 of a $1,400 crown and you pay the remaining $700 from an FSA, you save about $150-$200 in taxes.
Appeal denied claims when you believe coverage should apply. Insurance companies sometimes deny claims incorrectly or require additional documentation. Your dentist can help by providing clinical notes, X-rays, or a letter explaining medical necessity. Many denials are overturned on appeal, especially when the denial reason is vague or seems to contradict policy language.
Author: Daniel Mercer;
Source: ladylesliebelize.com
Consider timing your enrollment. If you know you need crown work and you're shopping for individual insurance, enroll as early as possible to start the waiting period clock. Some people enroll in a plan, wait out the 6-12 month waiting period while maintaining good oral hygiene, then schedule the crown work once coverage begins.
While "dental insurance that covers crowns 100 percent" sounds appealing, such plans are extremely rare in the individual market. Some employer plans offer 80% coverage for major services, but 100% crown coverage typically only exists in premium executive benefit plans or as a special feature after many years with the same carrier. Most people should expect to pay at least 50% out of pocket for crown work.
Frequently Asked Questions About Dental Crown Insurance Coverage
Crown coverage through dental insurance provides valuable financial assistance for these common restorative procedures, but rarely covers the full cost. Most plans classify crowns as major services with 50% coverage, annual maximum limits of $1,500-$2,000, and waiting periods of six to twelve months for new policies.
Your actual coverage depends on multiple factors: whether the crown is medically necessary, your plan type, the crown material, and your specific policy's limitations and exclusions. Understanding these variables before you need crown work helps you make informed decisions and avoid unexpected bills.
The key to maximizing your benefits lies in strategic planning—timing procedures to use multiple plan years, getting pre-treatment estimates, using in-network providers, and combining insurance with tax-advantaged accounts like FSAs or HSAs. While finding dental insurance that covers crowns 100% is unrealistic for most people, careful plan selection and smart utilization can significantly reduce your out-of-pocket costs for necessary crown work.
Related Stories

Read more

Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.




