
Two dental insurance policy documents on a wooden desk next to a dental mirror and toothbrush, soft natural lighting
Can You Have Two Dental Insurance Plans?
Yes, you can have two dental insurance plans at the same time. Many Americans find themselves with dual dental coverage through a combination of employer-sponsored plans, spousal benefits, or individual policies. While having two plans doesn't automatically mean double the benefits, it can reduce your out-of-pocket costs for expensive dental procedures when structured correctly.
The real question isn't whether you can have two plans—it's whether you should. Understanding how dual coverage works, what it actually costs, and when it makes financial sense requires looking beyond the surface appeal of "more coverage equals better coverage."
How Dual Dental Insurance Coverage Works
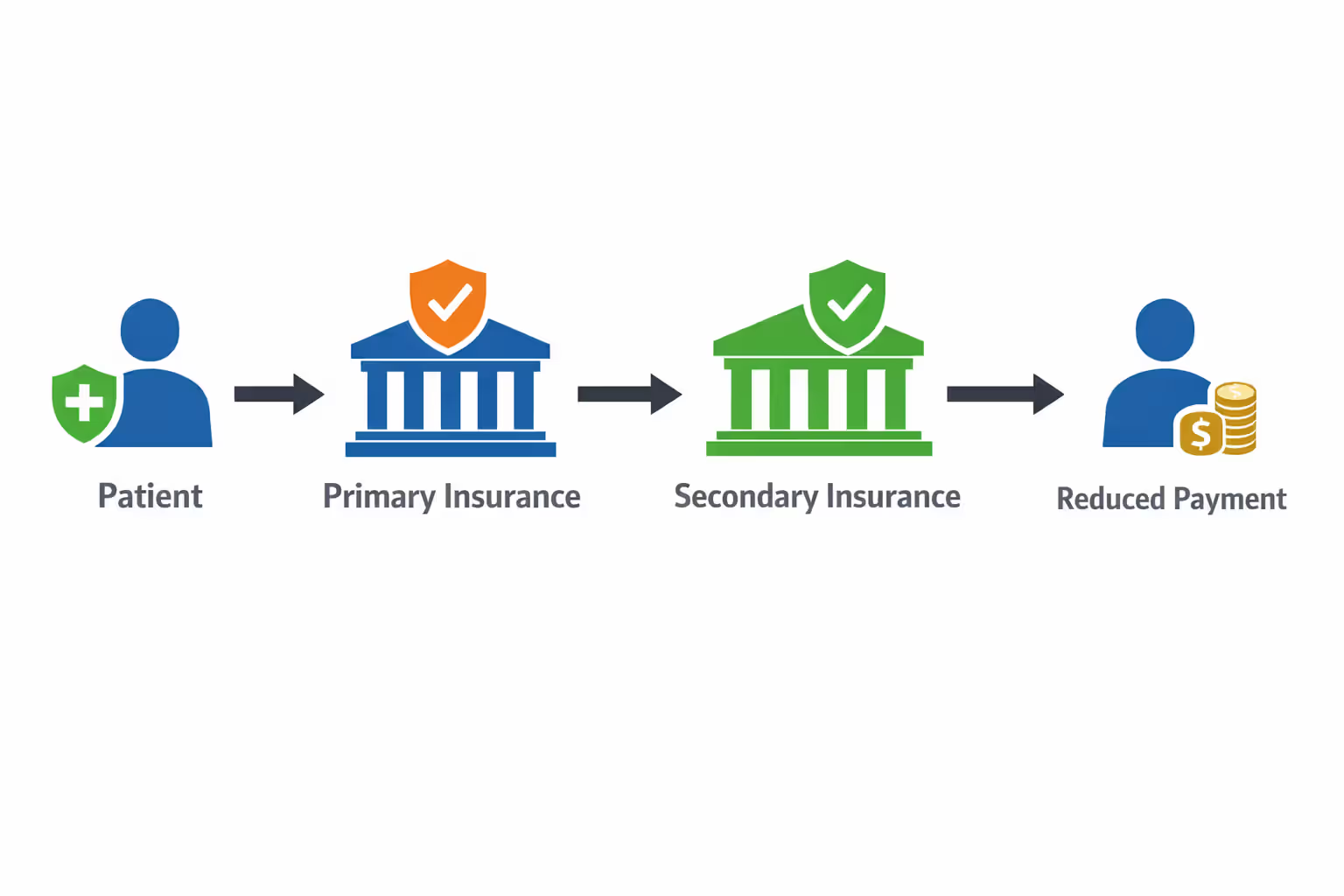
When you have two dental insurance policies, one becomes your primary plan and the other serves as secondary coverage. The primary insurance processes claims first, paying its portion according to the plan's terms. Your secondary insurance then reviews what remains and may cover some or all of the balance, up to its own limits.
The coordination of benefits (COB) process determines which plan pays first. For coverage through your own employer, that plan typically serves as primary. If you're covered under a spouse's plan as well, your employer plan remains primary for your care. For dependent children covered under both parents' plans, the "birthday rule" usually applies—the parent whose birthday falls earlier in the calendar year has the primary plan.
Insurance companies communicate during COB to prevent overpayment. You cannot collect more than 100% of covered expenses, even with two plans. If your primary insurance pays 80% of a crown, your secondary might cover part of the remaining 20%, but you won't receive duplicate payments.
Author: Tyler Grant;
Source: ladylesliebelize.com
Claims submission follows a specific order. You file with your primary insurer first, receive an Explanation of Benefits (EOB) showing what they paid, then submit that EOB along with the original claim to your secondary insurer. Some dental offices handle this coordination, but many require you to manage secondary claims yourself—adding administrative work to your plate.
The process differs from simply having more coverage. Both plans maintain their own annual maximums, deductibles, and coverage percentages. Your secondary plan won't necessarily fill every gap left by your primary coverage.
Situations Where Having Two Dental Plans Makes Sense
Dual coverage makes the most financial sense when you're facing expensive dental work that would exceed a single plan's annual maximum. Most dental insurance plans cap benefits between $1,500 and $2,000 per year. If you need multiple crowns, a bridge, or extensive periodontal treatment, two plans can help you avoid large out-of-pocket expenses.
Spousal employer coverage creates the most common dual insurance scenario. When both partners receive dental benefits through their jobs, each can maintain their own coverage as primary and add their spouse as a dependent on their plan. This arrangement works particularly well for families with children who need orthodontics or other major dental work.
Divorce situations sometimes result in temporary dual coverage, especially for children. Court orders may require both parents to maintain dental insurance, giving kids access to two plans during their formative years when orthodontic treatment is common.
Medicare beneficiaries often combine a Medicare Advantage plan that includes dental benefits with a standalone dental policy. Since traditional Medicare doesn't cover routine dental care, retirees sometimes layer coverage to manage costs during their higher-need years.
Specific coverage gaps also justify dual plans. If your employer plan excludes orthodontics or has a restrictive missing tooth clause, adding a secondary policy that covers these areas can be strategic—though you'll need to verify the second plan doesn't have similar exclusions.
Pros and Cons of Carrying Two Dental Insurance Policies
Benefits of Dual Coverage
Lower out-of-pocket costs for major procedures represent the primary advantage. When your primary plan pays 50% of a $2,000 crown and your secondary covers another 30%, you're left with $400 instead of $1,000.
Higher effective annual maximums give you more coverage for extensive treatment. Instead of hitting a $1,500 cap with one plan, you might access $2,500 to $3,000 in combined benefits—though this depends on how your secondary plan coordinates.
Better coverage for family members spreads benefits across more people. Parents often find dual coverage valuable when multiple children need dental work in the same year, effectively doubling the family's total available benefits.
Reduced wait times for certain procedures can occur if one plan has no waiting period for services the other restricts. You might use your secondary plan as primary for specific treatments if it offers better immediate coverage.
Drawbacks and Limitations
Premium costs often outweigh benefits for people with minimal dental needs. Paying $40-$60 monthly for a second plan means spending $480-$720 annually before receiving any benefit. If you only need preventive care, one plan typically suffices.
Administrative complexity increases significantly with dual coverage. You'll track two sets of ID cards, manage separate claims, follow up with multiple customer service departments, and understand two different benefit structures.
Coverage overlaps create inefficiency. Both plans might cover preventive care at 100%, meaning your secondary plan provides zero additional value for cleanings and exams—the services you'll use most frequently.
Coordination delays can slow reimbursement. Instead of one claim processed in two weeks, you might wait a month or longer while insurers communicate and process secondary claims.
Annual maximums don't always stack favorably. Some secondary plans only pay up to their own maximum minus what the primary paid, not the full secondary maximum. A $1,500 secondary maximum might only provide $500 in additional coverage if your primary already paid $1,000.

Author: Tyler Grant;
Source: ladylesliebelize.com
What Dual Dental Insurance Typically Covers and Doesn't Cover
Understanding coverage percentages helps set realistic expectations. Most dental plans follow a 100-80-50 structure: 100% coverage for preventive care (cleanings, exams, X-rays), 80% for basic procedures (fillings, simple extractions), and 50% for major work (crowns, bridges, dentures, root canals).
With dual coverage, your secondary plan applies its percentages to what remains after primary payment. If your primary pays 50% of a $1,200 crown ($600), your secondary doesn't automatically pay its 50% of the original charge. Instead, it considers the remaining $600 and applies its coverage rules—which might mean paying 50% of that balance ($300), leaving you with $300 out-of-pocket.
Annual maximums remain separate but don't simply double your coverage. Your primary plan's $1,500 maximum pays first. Your secondary plan's $2,000 maximum only applies to remaining balances, and many secondary plans reduce their payout based on primary payments.
Waiting periods apply to both plans independently. If you enroll in a second plan that has a 12-month waiting period for major services, you can't use it for crowns or bridges during that first year—even if your primary plan covers them immediately.
Missing tooth clauses affect both policies. Most dental insurance won't cover replacement of teeth missing before you enrolled. Asking "which dental insurance does not have a missing tooth clause" reveals that few plans omit this exclusion entirely. Some Medicare Advantage plans and certain state employee plans offer more flexibility, but these remain exceptions. Having two plans with missing tooth clauses doesn't override this limitation.
Orthodontic coverage requires special attention. Many plans exclude adult orthodontics or cap lifetime benefits at $1,000-$1,500. Dual coverage can increase available orthodontic benefits, but you'll need to verify both plans cover orthodontics and understand how they coordinate these specialized benefits.
Alternatives to Having Two Dental Insurance Plans
Discount dental plans offer an option worth considering before adding a second insurance policy. These membership programs (costing $100-$200 annually) provide 10-60% discounts on dental services at participating providers. While not insurance, they can reduce costs for people who need occasional major work without the premium expense of dual coverage.
Health insurance dental riders sometimes include limited dental coverage, particularly for accident-related dental injuries. Checking whether your medical insurance covers any dental services might reveal unexpected benefits. Some health savings account (HSA) compatible plans allow you to use pre-tax HSA funds for dental expenses, effectively discounting your costs by your tax rate.
Standalone supplemental dental plans specifically designed to fill gaps in primary coverage cost less than full second policies. These plans might focus on orthodontics, major procedures, or higher annual maximums while keeping premiums lower than comprehensive coverage.
Flexible spending accounts (FSA) and health savings accounts let you pay dental expenses with pre-tax dollars. Contributing $1,500 to an FSA effectively gives you a 22-32% discount (depending on your tax bracket) without any insurance premium. For people with predictable dental expenses, this approach often beats paying for a second insurance plan.
Direct payment arrangements with dentists can reduce costs more than insurance in some cases. Many dental practices offer 5-10% discounts for cash payment or provide in-house payment plans for major work. Building a relationship with a dentist who offers these options might serve you better than juggling two insurance policies.
Dental schools provide quality care at reduced rates—typically 30-50% below market prices. While appointments take longer because students perform the work under supervision, this option can make expensive procedures affordable without additional insurance.

Author: Tyler Grant;
Source: ladylesliebelize.com
How to Verify Your Current Dental Insurance Coverage
Start with your insurance ID card, which lists the insurance company name, your policy number, and a customer service phone number. The card might also show your group number, which you'll need when calling about benefits.
Contact your HR department if you receive coverage through an employer. Benefits administrators can explain your coverage details, provide summary plan descriptions, and clarify whether your plan coordinates with other insurance.
Call your insurance company directly using the number on your ID card. Ask specific questions: What's my annual maximum? What percentage does the plan cover for crowns? Do I have a deductible? Is there a waiting period for major services? Do you cover orthodontics? How does coordination of benefits work?
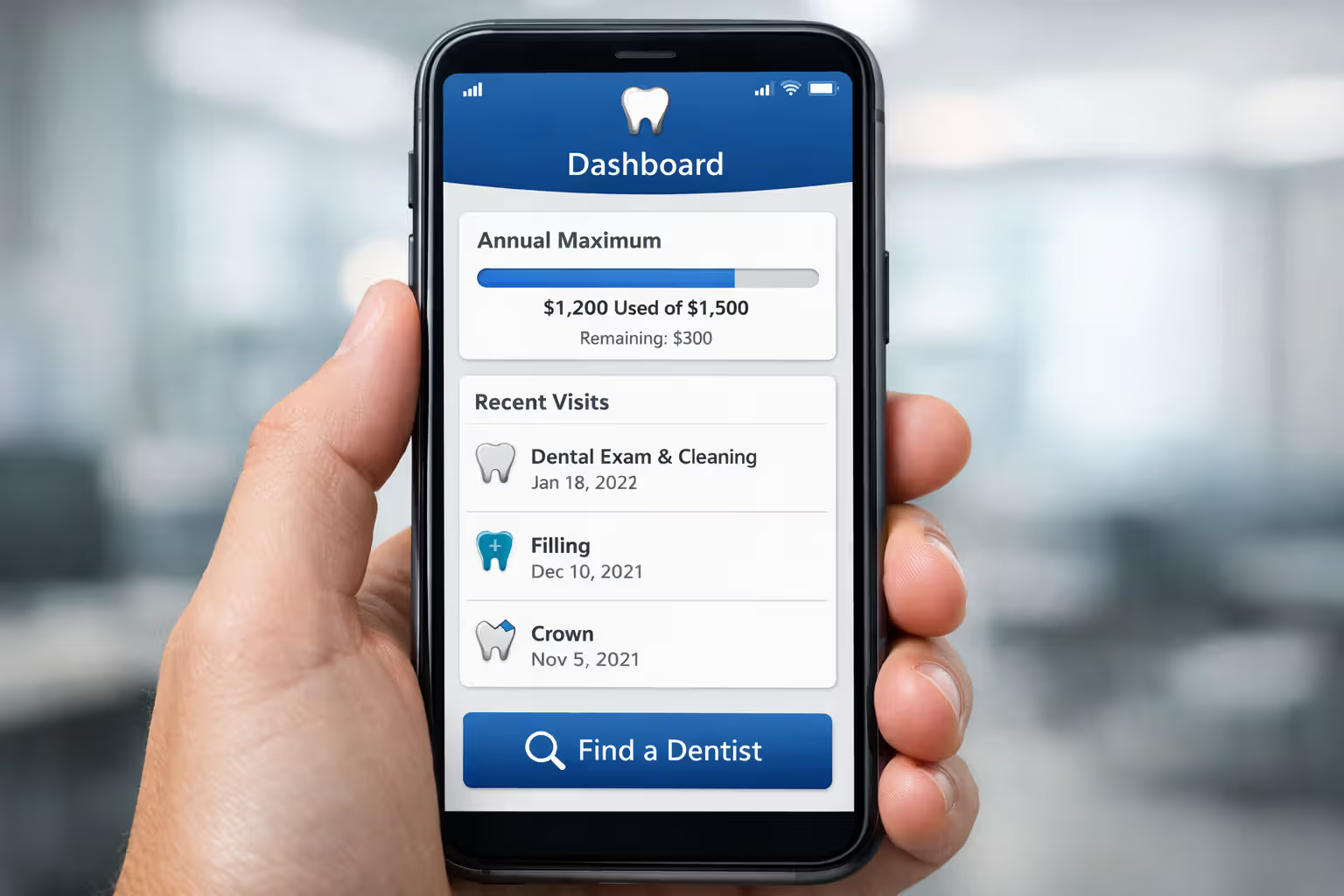
Log into your insurer's online portal to review your benefits summary, check your remaining annual maximum, view claims history, and find in-network providers. Most major dental insurers offer mobile apps with similar functionality.
Author: Tyler Grant;
Source: ladylesliebelize.com
Review your Explanation of Benefits (EOB) statements after dental visits. These documents show what your insurance paid, what you owe, and how much of your annual maximum remains. EOBs also reveal your coverage percentages for different service categories.
Request a pre-authorization for expensive procedures before scheduling treatment. Submit a treatment plan from your dentist to your insurance company, which will provide a breakdown of expected coverage. This step prevents surprises and helps you decide whether pursuing secondary coverage makes financial sense.
Ask your dentist's office to verify your benefits. Most dental practices check insurance coverage before major procedures and can explain what your plan will pay. However, verify this information independently—dental offices occasionally misunderstand coverage details.
When and How to Sign Up for Dental Insurance
Open enrollment periods restrict when you can enroll in employer-sponsored dental insurance. Most companies offer a 2-4 week window in late fall (typically November or December) when employees can add, change, or drop coverage effective January 1. Missing this window means waiting until the next year unless you experience a qualifying life event.
Qualifying life events allow mid-year enrollment changes. Marriage, divorce, birth or adoption of a child, loss of other coverage, or a change in employment status trigger special enrollment periods—usually 30-60 days from the event. You'll need to provide documentation proving the qualifying event occurred.
Individual marketplace dental plans sold through state exchanges or directly from insurers typically allow year-round enrollment. Unlike medical insurance, dental coverage doesn't have strict enrollment periods in the individual market. You can purchase a plan any month, though your effective date might be the first of the following month.
Employer plan enrollment requires submitting elections through your company's benefits portal or HR department during open enrollment. You'll choose between plan options (if multiple are offered), decide whether to cover dependents, and authorize payroll deductions for premiums.
Standalone dental insurance purchased directly from insurers involves comparing plans online or working with an insurance broker. Look for plans that fit your needs—don't just choose the lowest premium. Consider annual maximums, coverage percentages, network size, waiting periods, and specific exclusions.
Medicare beneficiaries can add dental coverage during Medicare's annual open enrollment (October 15-December 7) by switching to a Medicare Advantage plan that includes dental benefits. Standalone Medicare dental plans can be purchased year-round.
Timing matters for maximizing dual coverage. If you're planning major dental work and want to add a second plan, enroll as early as possible to satisfy any waiting periods. Some people strategically time procedures to span two calendar years, using one year's maximum from each plan.
Many people assume that having two dental plans means they'll pay nothing out-of-pocket, but coordination of benefits doesn't work that way. The secondary plan looks at what the primary already paid and determines its obligation based on that. I've seen clients pay for a second plan for years without using it because they only needed cleanings and basic fillings—services their primary plan already covered well. Dual coverage makes sense when you're facing major dental work that would exceed one plan's annual maximum, but it's not a magic solution for everyone
— Sarah Mitchell
Frequently Asked Questions About Dual Dental Coverage
Deciding whether to maintain two dental insurance plans requires honest assessment of your dental health, anticipated needs, and financial situation. Calculate the annual cost of premiums for a second plan against the potential savings on procedures you're likely to need. For someone with healthy teeth who visits the dentist twice yearly for cleanings, dual coverage rarely makes financial sense.
Families facing orthodontics, individuals needing multiple crowns or bridges, or people with ongoing periodontal disease represent the clearest cases for dual coverage. When your dental expenses will exceed $3,000-$4,000 in a year, the premium cost of a second plan typically pays for itself through reduced out-of-pocket costs.
Consider alternatives before committing to dual insurance. Discount dental plans, FSAs, and payment plans with your dentist might deliver better value with less complexity. If you do pursue dual coverage, understand the coordination of benefits process, keep detailed records, and maintain clear communication with both insurers.
The question isn't just whether you can have two dental insurance plans—you absolutely can. The real question is whether the added coverage justifies the premium cost and administrative burden for your specific situation. Run the numbers, consider your dental health trajectory, and make the choice that aligns with both your mouth and your budget.
Related Stories

Read more

Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.




