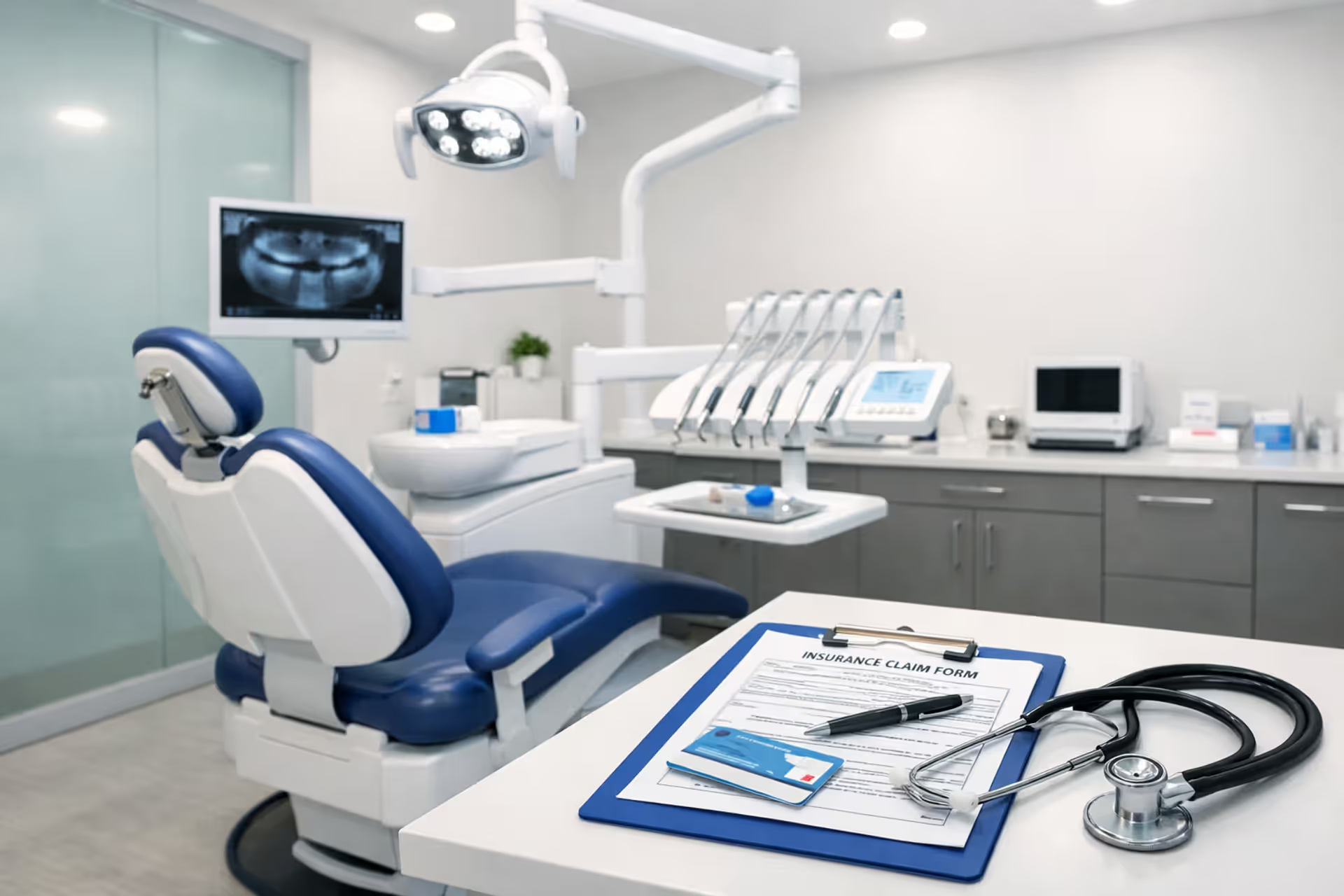
A clean infographic timeline showing 12 months of the year with color-coded dental insurance enrollment windows for employer plans, ACA marketplace, Medicare, and private individual plans
Can You Get Dental Insurance Anytime
My friend Sarah called me last Tuesday morning in full panic mode. She'd woken up with half a molar missing and assumed she could buy dental coverage before her emergency appointment at 2 PM. Twenty minutes of frantic googling later, she discovered the truth: dental insurance doesn't work that way. At all.
Most Americans think buying dental coverage works like shopping for car insurance—something you can do whenever the need strikes. The reality involves enrollment windows, qualifying events, waiting periods that stretch for months, and payment structures that vary wildly between dental offices. Getting these details wrong costs people hundreds or thousands of dollars every single day.
When You Can Enroll in Dental Insurance
The answer to "can I sign up right now" shifts dramatically based on where the coverage originates. Each source operates under completely different rulebooks.
Employer-Sponsored Plans
Most companies offer a brief enrollment window each autumn—typically three to four weeks somewhere between mid-October and late November. During this period, you're making binding decisions about coverage for the entire following calendar year. Miss this window and you're locked out until next fall unless your life circumstances change significantly.
What qualifies as a significant change? Marriage opens a special enrollment period. Having or adopting a child does too. Divorce, legal separation, death of a spouse, losing coverage you previously had through another source, or switching between full-time and part-time employment status all create opportunities to adjust your benefits mid-year. HR departments typically grant you 30 days after the qualifying event to complete paperwork—occasionally 60 days at more generous employers. Wait longer and that window slams shut.
Here's something that catches people off-guard: some companies separate medical and dental enrollment completely. I've watched small businesses allow new hires to add dental coverage anytime during month one while requiring day-one enrollment decisions for medical plans. Your HR representative can clarify these specific timelines—don't assume dental follows the same rules as health insurance.
ACA Marketplace Plans
The federal marketplace at healthcare.gov offers standalone dental products completely separate from medical coverage. Enrollment runs approximately ten weeks annually, from November 1st through mid-January (the exact closing date shifts slightly year to year).
What surprises many people: carrying medical insurance through your employer doesn't prevent you from purchasing separate dental coverage through the marketplace. These products don't conflict. You're still bound by that November-to-January enrollment window, though, unless a qualifying life event grants you a special enrollment opportunity.
Author: Daniel Mercer;
Source: ladylesliebelize.com
Private Individual Plans
This category finally delivers the "yes, purchase whenever you want" answer people are searching for. Carriers like Delta Dental, Humana, Renaissance, and Cigna accept applications twelve months a year. March, July, December—makes no difference to them. No enrollment periods restrict when you can buy.
The tradeoff hits hard, though. Waiting periods before coverage activates can be punishing. Basic preventive services like cleanings? Often available immediately. That filling causing you pain? Expect a three-month delay before coverage begins. Crown work? Six to twelve months of waiting is standard. Desperately need a root canal in fourteen days? Purchasing a policy this afternoon won't help you in time.
Medicare Dental Coverage
Traditional Medicare provides zero dental benefits. Medicare Advantage plans sometimes bundle dental coverage into their packages, but enrollment is restricted to three annual windows: the fall open enrollment from October 15 through December 7, the Medicare Advantage disenrollment period from January 1 through March 31, plus your initial eligibility window when you first qualify for Medicare at age 65. Outside these windows, you're waiting for the next opportunity. Seniors can purchase standalone private dental policies year-round, though once again, waiting periods apply before coverage activates for anything beyond basic cleanings.
| Plan Type | When You Can Enroll | Restrictions That Apply | Can You Sign Up Today? |
| Employer coverage | Typically 3-4 weeks each autumn | Must wait for open enrollment unless qualifying life event occurs | Unlikely unless currently in enrollment window |
| Healthcare.gov marketplace | November 1 through mid-January annually | Restricted to enrollment period except after qualifying events | Only during November-January timeframe |
| Direct purchase from insurance carriers | Every day of the year | Waiting periods delay coverage activation (typically 3-12 months) | Yes, though benefits won't start immediately |
| Medicare Advantage including dental | Oct 15–Dec 7, Jan 1–Mar 31, initial eligibility window | Limited to specific enrollment periods | Only during designated months |
How Dental Insurance Payment Works
The "do you pay the full amount upfront" question confuses people because individual dental practices handle this completely differently. I've walked out of preventive appointments paying nothing. I've paid estimated amounts that required later adjustment. One orthodontist insisted on full payment upfront and left me to battle the insurance company for reimbursement myself.
Direct Payment vs. Reimbursement Models
Dentists who participate in your insurance network typically file claims on your behalf. You pay whatever portion they calculate you owe at checkout—sometimes zero for preventive services, perhaps 20% for basic restorative work, maybe 50% for major procedures. The practice submits your claim, receives payment from your insurance carrier weeks later, then either refunds you money or sends an additional bill once the actual claim processes and they discover what you truly owed.
Other dentists—particularly specialists, cosmetic practitioners, or providers who refuse to participate in insurance networks—demand full payment when they complete your treatment. You write a check for the entire $1,800 crown cost, file the insurance paperwork yourself, then wait weeks for a reimbursement check to arrive. This model appears less frequently now than a decade ago, but it hasn't disappeared entirely.
What You Actually Pay at the Appointment
Preventive services like routine cleanings and periodic exams often cost you nothing out-of-pocket when your plan covers them at 100% without applying your deductible. Basic procedures including fillings typically require you to cover 20-40% of the contracted rate. Major work—crowns, bridges, dentures—frequently splits 50/50 between you and your insurance.
Here's where confusion multiplies: the front desk collects an estimate when you check out. They're making an educated prediction based on your insurance card details and their experience with similar claims. Two to six weeks later, after your actual claim finishes processing, that estimate might prove wildly inaccurate.
Real situation from six months ago: my coworker scheduled a crown. The front desk quoted her $450 as her share of a $1,350 procedure covered at 50%. She paid $450 that day. Almost six weeks passed before she received a bill demanding another $315. Turns out she'd already burned through $1,385 of her $1,500 annual maximum on earlier procedures, leaving only $115 of insurance money available for this crown. Nobody caught the error until the claim fully processed through the system.

Author: Daniel Mercer;
Source: ladylesliebelize.com
Deductibles and Annual Maximums
Most dental coverage requires you to pay the first $50-100 of costs each calendar year before your plan contributes anything toward basic or major services. This deductible rarely applies to preventive care—checkups and cleanings usually bypass it entirely.
Annual maximums reveal how outdated dental insurance design has become. Plans typically cap their contribution at $1,000-2,000 per year. Once your carrier has paid that amount, you're responsible for 100% of any additional costs until January 1st rolls around. These maximums haven't increased meaningfully since the 1970s while dental costs have roughly tripled. A $1,500 maximum purchased significantly more dental care three decades ago than it does today.
Having Multiple Dental Insurance Plans
Carrying multiple dental policies is absolutely permitted. Plenty of people do exactly that—perhaps you've secured coverage through your job while your spouse obtained coverage through theirs. The real question isn't whether you're allowed to maintain two plans simultaneously, but whether that second policy will actually contribute money after the first plan processes your claim.
Coordination of benefits rules prevent double-dipping. Insurance carriers communicate behind the scenes to verify they're not collectively reimbursing more than 100% of your dentist's actual charges. You can't profit financially from dental treatment by stacking multiple policies.
Your first plan pays according to its standard coverage structure. The second plan may cover part or all of what remains unpaid, though you'll never receive reimbursement exceeding the total treatment cost.
How Primary and Secondary Coverage Coordination Works
Established regulations determine which carrier pays first. When you're covered both through your own employer and through your spouse's employer, your own employer's coverage becomes primary for your claims every time. Your spouse's employer plan serves as secondary.
Children covered under both parents' employer plans typically follow the "birthday rule"—whichever parent has a birthday earlier in the calendar year (not who's older chronologically, just whose birthday comes first from January through December) provides the primary coverage. Dad's birthday falls on March 12th and mom's birthday is September 3rd? Dad's insurance becomes primary for the kids' dental claims.
Watch how this calculation works in practice:
Scenario: You require a $1,200 crown. Your primary coverage pays 50% on major work after a $50 deductible. Your secondary plan pays 50% on major work with no deductible requirement.
- Primary insurance calculates: $1,200 minus $50 deductible equals $1,150, then pays 50% which equals $575
- Amount you still owe: $625
- Secondary insurance examines the original $1,200 charge, determines it would normally contribute 50% ($600), notices only $625 remains unpaid, so pays $600
- Your final cost: $25 (only the primary deductible that the secondary plan didn't cover)
Without that secondary coverage, you'd be paying $625. With both plans coordinating, you're paying $25.
| Situation | Primary Plan Contribution | Secondary Plan Contribution | Your Final Cost | Dentist's Total Charge |
| $1,200 crown with single plan (50% coverage, $50 deductible) | $575 | Nothing | $625 | $1,200 |
| Same crown with dual coverage (both at 50%) | $575 | $600 | $25 | $1,200 |
| $150 preventive cleaning with single plan (100% coverage) | $150 | Nothing | $0 | $150 |
| Same cleaning with dual coverage | $150 | $0 (nothing remains to pay) | $0 | $150 |
Can You Have Three Dental Insurance Plans
Technically speaking? Sure, nothing legally prevents it. From a practical standpoint? Almost never worth the hassle.
You remain limited to 100% reimbursement of covered charges through coordination of benefits regardless of how many policies you maintain. A third policy would only contribute if policies one and two combined failed to cover everything. Meanwhile you're paying premiums on three separate plans, submitting paperwork for three different claims on every single procedure, and tracking three distinct coverage periods and annual maximums.
One extremely narrow scenario where three plans might provide value: you've exhausted the annual maximums on plans one and two, and plan three exclusively covers services the other two specifically exclude. Maybe the third plan covers orthodontia while your first two plans don't. Even in this situation, calculate whether the premiums for that third plan exceed the cost of simply paying out-of-pocket.
For 99% of people, three policies creates triple the administrative burden for essentially zero additional financial benefit.
Getting Insurance Coverage for Dental Implants
Dental implants exist in a frustrating coverage gray area. Traditional dental insurance frequently classifies implant procedures as cosmetic treatment and denies coverage outright. Plans that do acknowledge implants usually categorize them as major services eligible for 50% coverage, which initially sounds helpful until you realize each implant costs $3,000-6,000 while your annual maximum hovers around $1,500. The insurance company contributes $750, leaving you responsible for thousands.
Strategies to Maximize Dental Insurance Coverage for Implants
Start by thoroughly reading your actual policy documents—not the two-page summary, the complete policy. Some employers competing aggressively for talent have begun including implant coverage in their benefits packages. Coverage varies dramatically when it exists, though 50% reimbursement after meeting your deductible represents the typical structure.
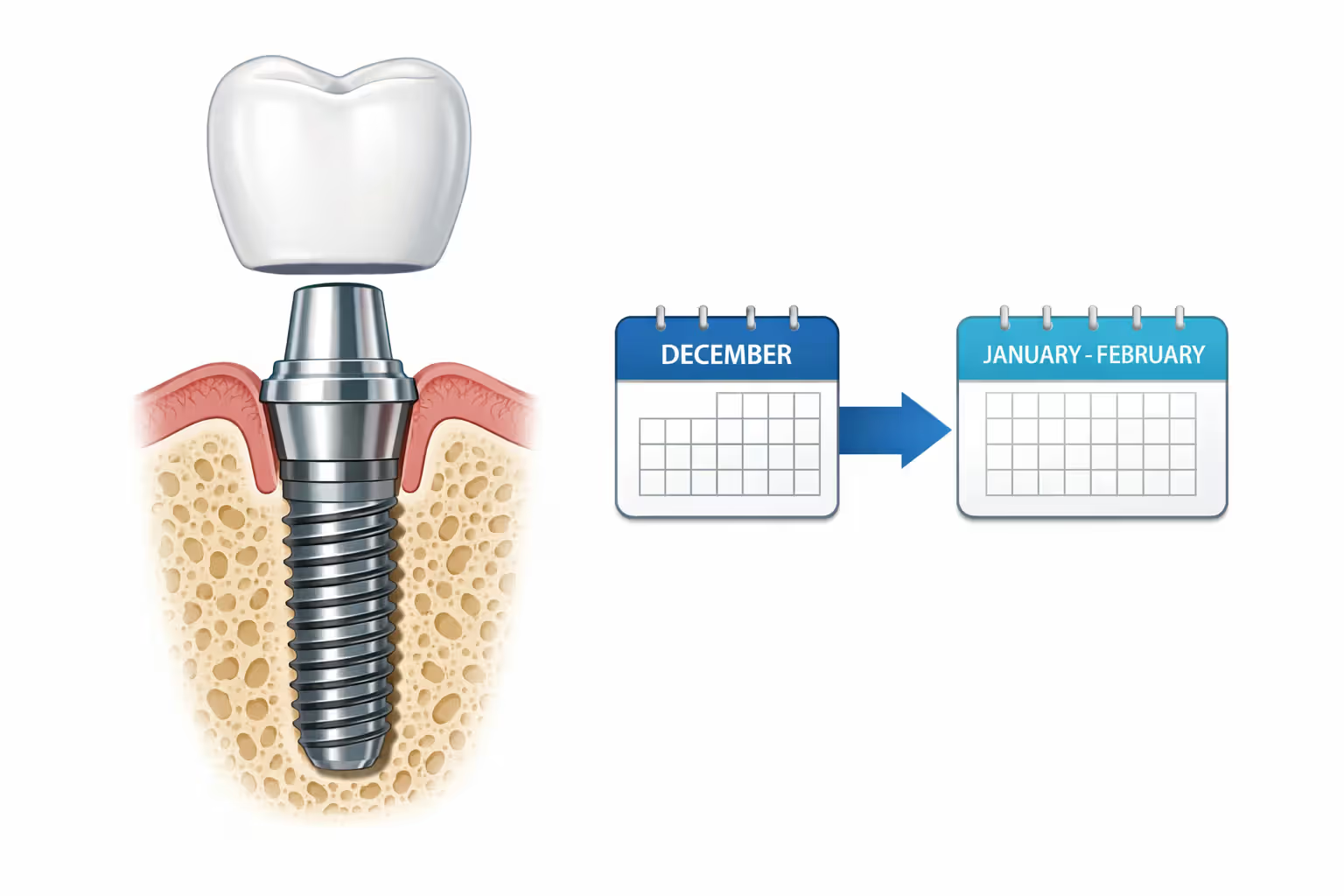
Strategic timing of procedures can effectively double your insurance benefit. Suppose your dentist recommends an implant in November and your plan renews each January 1st. Split the work across two calendar years. Extract the damaged tooth and complete the bone graft in December, using this year's $1,500 maximum. Place the implant post in January and add the crown in February, accessing next year's $1,500 maximum. You've transformed $1,500 of insurance contribution into $3,000 by waiting approximately six weeks. Your dentist must agree to work within this timeline, and your oral health must allow the delay.
Author: Daniel Mercer;
Source: ladylesliebelize.com
Obtain pre-authorization before any work begins. Insurance carriers want to review implant cases and approve coverage before treatment starts. Your dentist submits X-rays, detailed treatment plans, and medical justification explaining why you need this implant for proper oral function rather than purely cosmetic reasons. The insurance company issues a determination—not an ironclad guarantee, but a written statement indicating what they'll likely pay. This process prevents devastating financial surprises after the procedure is complete.
Financing plans through CareCredit or similar medical credit services let you spread the uncovered portion over 12-24 months, often interest-free if you maintain the payment schedule. This approach doesn't reduce your total cost, but transforms a $3,500 bill into manageable $175 monthly payments.
When Medical Insurance May Cover Dental Procedures
Medical insurance covering dental treatment is uncommon, but it does happen under specific circumstances. The critical distinction: did a medical condition or accident cause the dental problem, or did ordinary dental disease create it?
Lost multiple teeth in a car accident? Medical insurance may cover implant placement as reconstructive surgery. Require teeth extracted before undergoing radiation therapy for cancer because the radiation will destroy them regardless? Medical insurance could cover those extractions as medically necessary cancer treatment preparation. Jaw tumor requiring tooth removal? Medical coverage applies.
Gum disease causing tooth loss? That's standard dental disease—medical insurance won't contribute. Cavity requiring crown work? Dental issue, not medical. Tooth cracks from grinding? Dental problem, even when stress triggers the grinding behavior.
Certain medical plans cover dental procedures performed in hospital operating rooms under general anesthesia, particularly for patients with severe developmental disabilities, autism spectrum disorders, or medical conditions making office-based dentistry dangerous. The facility fees and anesthesiologist charges might qualify under medical benefits even though the dental work itself doesn't.
Filing medical insurance claims for dental procedures demands extensive documentation. Your dentist and physician both must provide detailed written explanations of why this dental work treats a medical condition rather than routine dental disease. Expect initial claim denials as standard practice. Plan to file appeals with supplemental records and additional justification. It's a bureaucratic marathon.
People assume medical insurance will cover dental emergencies or expensive implant procedures without actually verifying coverage beforehand. Medical policies have incredibly narrow criteria for dental work coverage. The typical implant replacing a tooth lost to decay or periodontal disease won't satisfy those criteria regardless of medical necessity. Always obtain written pre-authorization before spending thousands based on assumptions about coverage
— Jennifer Martinez
Common Enrollment Mistakes to Avoid
Missing Qualifying Event Deadlines
Special enrollment windows close quickly. Get married on June 15th? Your deadline to add your spouse to dental coverage probably falls around August 14th—exactly 60 days later. Wait until August 20th and you're stuck until October's open enrollment. Set phone calendar reminders and submit required paperwork within days of the qualifying event, not weeks later when you finally find time.
Ignoring Waiting Periods
Purchasing private dental insurance the afternoon before your scheduled root canal accomplishes nothing except wasting premium dollars. Waiting periods exist specifically to prevent people from buying coverage only when facing expensive treatment needs. Root canal coverage won't activate for six months minimum, frequently a full year. Some carriers waive waiting periods if you can prove continuous prior coverage with zero gaps, though you'll need formal documentation from your previous insurance company.
Choosing Plans Based Solely on Premium
A $15 monthly premium looks dramatically better than a $40 monthly premium. But suppose the cheaper plan caps annual coverage at $750 while the expensive plan offers $2,000 maximum coverage—which actually costs you less? Calculate the complete math. If you need $2,200 in dental work annually:
- Cheap plan: ($15 × 12 months) + ($2,200 - $750 coverage) = $180 + $1,450 = $1,630 total annual cost
- Expensive plan: ($40 × 12 months) + ($2,200 - $2,000 coverage) = $480 + $200 = $680 total annual cost
The "expensive" plan saves you almost $950 despite higher monthly premiums. Always calculate total annual costs—premiums plus anticipated out-of-pocket expenses based on your realistic dental needs—rather than focusing exclusively on monthly premium amounts.

Author: Daniel Mercer;
Source: ladylesliebelize.com
Forgetting to Update Coverage After Life Changes
You dropped your individual dental plan after getting married and joining your spouse's employer coverage three years ago. Now you're divorcing. Assuming your ex-spouse's HR department will notify you when coverage terminates is a dangerous mistake. Without arranging replacement coverage during your 60-day special enrollment window, you could spend months completely uninsured. Divorce decrees should specify insurance transition responsibilities, but they frequently don't address this critical detail.
Not Verifying Provider Networks
Your trusted dentist of 15 years might not participate in your new insurance network. Out-of-network care costs substantially more—some plans provide zero coverage for non-participating providers. Before enrolling in any plan, call your dentist's office directly and ask specifically whether they accept the plan you're considering. Never rely on online provider directories, which are notorious for containing outdated information. Confirm by telephone with the actual practice, or be prepared to find a different dentist.
FAQ About Dental Insurance Enrollment and Coverage
Dental insurance operates less flexibly than most people anticipate. You cannot simply decide you want coverage and enroll immediately unless you're purchasing a private individual plan—and even those impose waiting periods delaying coverage activation for months. Employer and marketplace plans restrict enrollment to narrow annual windows, making timing absolutely essential.
Understanding payment procedures before your first appointment prevents awkward surprises at the front desk. Knowing how multiple policies coordinate saves significant money if you're fortunate enough to carry dual coverage. For expensive procedures like implants, researching your specific plan's regulations, obtaining pre-authorization in writing, and strategically timing treatment across calendar years can save thousands of dollars.
The most common enrollment mistakes—missing deadlines, ignoring waiting periods, selecting plans based exclusively on premium costs without calculating total annual expenses—are completely preventable with careful attention to detail and advance planning.
Before enrolling in any dental plan, calculate your anticipated total annual costs including both premiums and expected out-of-pocket expenses based on your realistic dental health needs. Confirm your preferred dentist participates in the network by calling their office directly. Understand precisely when coverage becomes effective and what waiting periods apply to different service categories. Read the complete policy documents, not just the marketing summary brochure.
Dental insurance lacks standardization. What works perfectly for your coworker might be terrible for your situation. The optimal enrollment timing and plan structure depend on your employment status, whether you can access coverage through a spouse, your family's dental health history, expected procedures, and budget constraints. Taking time to understand these variables before you face a dental emergency puts you in control of both your oral health and your financial planning.
Related Stories
Read more

Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer guidance on dental insurance topics, including coverage options, premiums, deductibles, waiting periods, annual maximums, claims processes, and procedures that may be covered by insurance such as implants, braces, crowns, dentures, and preventive care. The information presented should not be considered medical, dental, financial, or professional insurance advice.
All articles and explanations published on this website are for informational purposes only. Dental insurance policies may vary between providers, and details such as coverage limits, exclusions, reimbursement rates, waiting periods, and eligibility requirements can differ depending on the insurer, plan, and individual circumstances.
While we strive to keep the information accurate and up to date, this website makes no guarantees regarding the completeness or reliability of the content. Use of this website does not create a professional relationship. Visitors should review official policy documents and consult with licensed dental or insurance professionals before making decisions regarding dental care or insurance coverage.